Superior Semicircular canal dehiscence (SSCD)
What is Superior Semicircular Canal Dehiscence?
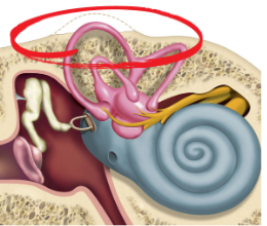
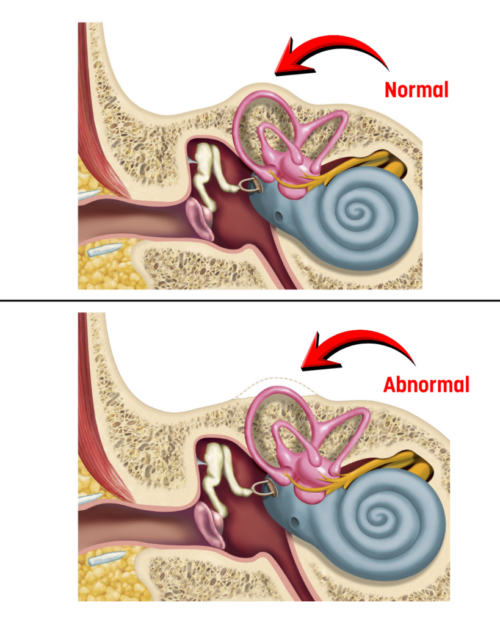
SSCD is a condition characterized by a defect (absence or thinning) in the bone overlying the superior semicircular canal, creating an abnormal opening in the bony labyrinth (Ward et al., 2021; Sood et al., 2017).
This opening acts as a “third mobile window,” in addition to the oval and round windows, and alters normal inner ear fluid mechanics (Ward et al., 2021). As a result, sound and pressure can be transmitted abnormally to the vestibular system, producing both auditory and vestibular symptoms (Ward et al., 2021).
In simple terms, SSCD is a small opening in the inner ear that makes it unusually sensitive to sound and pressure, which can sometimes lead to dizziness and unusual hearing sensations.

History
- First described in 1998 by Dr. Lloyd B. Minor and colleagues
- Early cases were often misattributed to conditions such as perilymph fistula before SSCD was recognized as a distinct disorder
- Advances in high-resolution temporal bone CT enabled reliable identification of the defect and broader recognition of the condition
- Diagnostic criteria were later standardized by the Bárány Society (2021), integrating symptoms, imaging, and physiologic testing

Dr. Lloyd B. Minor
Etiology
It is thought to result from thinning or absence of bone over the superior semicircular canal, leaving the area vulnerable to developing a dehiscence (Ward et al., 2021; Castellucci et al., 2014). Some literature suggests this may reflect incomplete bone formation, with the overlying bone remaining thin and susceptible to breakdown over time rather than a fully formed defect at birth (Castellucci et al., 2014).
The dehiscence may then develop or become symptomatic later due to factors such as mechanical stress or pressure-related changes (Sood et al., 2017; Castellucci et al., 2014). Overall, SSCD is considered multifactorial and not fully understood.
Prevalence
SSCD is considered uncommon, and its true prevalence is difficult to determine. Temporal bone studies suggest superior canal dehiscence is present in approximately 0.7% of individuals, with an additional 1.3% demonstrating markedly thin bone over the canal (Carey et al., 2000).
Imaging studies have reported higher rates of apparent dehiscence, likely reflecting radiologic overestimation, with CT-based prevalence reported up to 4% or higher (Cloutier et al., 2008). However, more recent high-resolution CT studies in asymptomatic individuals suggest a prevalence closer to ~2%, supporting the presence of false positives on imaging alone (Berning et al., 2019).
Because radiologic dehiscence may be identified in asymptomatic individuals, the prevalence of symptomatic SSCD is likely lower than the prevalence of anatomic or radiologic dehiscence (Ward et al., 2021).
SSCD Diagnostic Criteria – Bárány Society
The diagnosis of superior semicircular canal dehiscence syndrome requires all of the following criteria:
- At least 1 of the following symptoms consistent with the presence of a ‘third mobile window’ in the inner ear:
-
-
Bone conduction hyperacusis
- Sound-induced vertigo and/or oscillopsia time-locked to the stimulus
-
Pressure-induced vertigo and/or oscillopsia time-locked to the stimulus
- Pulsatile tinnitus
-
2. At least 1 of the following signs or diagnostic tests indicating a ‘third mobile window’ in the inner ear:
-
- Nystagmus characteristic of excitation or inhibition of the affected superior semicircular canal evoked by sound, or by changes in middle ear pressure or intracranial pressure
- Low-frequency negative bone conduction thresholds on pure tone audiometry
- Enhanced VEMP responses (low cervical VEMP thresholds or high ocular VEMP amplitudes)
3. High resolution temporal bone CT imaging with multiplanar reconstruction demonstrating dehiscence of the superior semicircular canal
4. Not better accounted for by another vestibular disease or disorder
Patient Reported Symptoms
Patients with SSCD may be:
- Completely asymptomatic
- Vestibular symptoms only
Dizziness, vertigo, oscillopsia, or imbalance, often triggered by sound or pressure - Hearing loss only
- Autophony or tinnitus only
- A combination of vestibular and auditory symptoms
Patients may report autophony, bone-conduction hyperacusis, tinnitus, hearing loss, dizziness, oscillopsia, or ongoing unsteadiness. Sound- and pressure-induced symptoms, such as those triggered by loud noises, coughing, sneezing, or straining, are characteristic of SSCD and help distinguish it from other vestibular disorders, although some patients also have spontaneous symptoms (Ward et al., 2021; Naert et al., 2018; Fritz et al., 2023).
Clinical Findings
Clinical findings in superior semicircular canal dehiscence (SSCD) are based on how the inner ear responds abnormally to sound and pressure.
🔍 Bedside Testing
These tests may help give an indication of SSCD by applying sound or pressure and observing the nystagmus that results. These findings are best seen using infrared video goggles, which allow subtle nystagmus to be detected.
- Valsalva maneuver (bearing down):
When the patient increases pressure in the chest or head (for example, as if trying to exhale with the nose pinched), this can stimulate the affected canal and produce vertical–torsional nystagmus and symptoms. The direction of the eye movement follows the plane of the superior semicircular canal, which helps localize the involved structure (Ward et al., 2021) - External auditory canal pressure (e.g., tragal pressure):
Gentle pressure applied to the ear canal can transmit mechanical force to the inner ear and provoke canal-specific nystagmus and/or symptoms. This reflects abnormal pressure transmission through the dehiscence (Ward et al., 2021) - Sound stimulation (Tullio phenomenon):
Loud sounds can directly activate the vestibular system, producing nystagmus aligned with the superior canal. This occurs because the third window allows sound energy to affect balance structures more than normal (Ward et al., 2021) - Skull vibration:
Applying vibration to the skull may provoke nystagmus by creating asymmetric stimulation between the ears. This can be helpful for identifying the affected side, although it is considered an adjunct test rather than a primary diagnostic tool (Dumas et al., 2024)
🧪 Objective Testing
In addition to bedside testing, several objective measures provide support for SSCD.
Vestibular Evoked Myogenic Potentials (VEMP):
Often over-responsive, with lower thresholds and larger amplitudes due to increased sensitivity from the third window (Ward et al., 2021; Castellucci et al., 2021).
Audiometry:
May show an air–bone gap despite normal middle ear function. Bone conduction thresholds can be unusually sensitive (better than 0 dB), consistent with third-window physiology (Ward et al., 2021; Naert et al., 2018).
vHIT:
Assesses the vestibulo-ocular reflex during rapid head movements. VOR gain in the superior canal may be mildly reduced, as the third window allows energy to dissipate, resulting in less effective cupula deflection. Findings are often subtle or variable and should be interpreted alongside other clinical data (Castellucci et al., 2021).
🖥️ Imaging
- High-resolution CT of the temporal bone is required to confirm the diagnosis
- Thin slice imaging (≤0.5 mm) with appropriate reformats improves the ability to accurately detect a dehiscence (Ward et al., 2021; Cloutier et al., 2008).
⚖️ Balance and Functional Findings
Balance testing in SSCD is often variable and non-specific.
Some individuals may demonstrate unsteadiness or gait instability, particularly in more complex or visually challenging environments. However, these findings are not consistent and are not used to diagnose SSCD (Naert et al., 2018; Ward et al., 2021).
In select or more complex cases, balance impairment may be more noticeable, but findings vary widely and are not well standardized across patients (Carender et al., 2018; Khalili et al., 2026).
👉 Overall, balance testing may help describe functional impact, but does not provide specific diagnostic information for SSCD.
Treatment
Management of superior semicircular canal dehiscence (SSCD) is guided by symptom severity and functional impact. Not all individuals with radiographic dehiscence require treatment.
🛑 Conservative Management
For individuals with symptoms that are mild, intermittent, or not functionally limiting, management is typically non-surgical.
- Education and trigger reduction:
Patients may benefit from identifying and limiting exposure to sound and pressure triggers (e.g., loud environments, straining), which are known to provoke abnormal vestibular responses in SSCD (Ward et al., 2021). -
Vestibular rehabilitation (VRT):
Vestibular therapy does not treat the underlying dehiscence, as it cannot correct the third-window lesion.However, it may be appropriate in specific situations, including:
- Persistent imbalance or functional limitations
- Postoperative recovery, when patients experience dizziness, gait instability, or reduced tolerance to movement
In these cases, rehabilitation focuses on:
- Improving balance and gait function
- Gradual reintroduction of movement to reduce activity limitation
- Promoting central compensation following altered vestibular input
Evidence for vestibular rehabilitation in SSCD is limited and primarily based on postoperative case-level data, rather than large controlled studies (Carender et al., 2018).
👉 Importantly, VRT is considered supportive, not corrective, in SSCD
🔧 Surgical Management
Surgical treatment is considered when symptoms are persistent, clearly linked to SSCD, and functionally limiting.
- Goal of surgery:
To eliminate the abnormal third-window effect and restore more normal inner ear mechanics - Surgical techniques:
- Canal plugging
- Resurfacing of the superior semicircular canal
- Surgical approaches:
- Middle cranial fossa
- Transmastoid
These techniques and approaches are well described in the literature, with selection based on anatomy, symptoms, and surgeon experience (Castellucci et al., 2014; Mekonnen et al., 2024).
📈 Outcomes
Surgical series report that many patients experience improvement in vestibular and auditory manifestations following repair, although outcomes vary and no single surgical technique has been shown to be universally superior (Mekonnen et al., 2024; Castellucci et al., 2014).
🔄 Postoperative Considerations
After surgery, patients may experience temporary vestibular hypofunction, BPPV, imbalance, or motion sensitivity.
- Vestibular rehabilitation may be used to:
- Treat BPPV with Canalith Repositioning Maneuvers
- Improve gait and balance stability
- Address persistent dizziness with movement
- Support return to daily activities
To Learn More — Check Out These Resources
- Vestibular First’s Online, self-paced CEU courses:
- Watch related Journal Clubs:
- FREE PDF Resources:
- FREE page:

References
- Ali L, Ali A, Salib S, Tehrani NS, Yang HH, Mozaffari K, Gopen Q. Headache resolution following the middle fossa repair of superior semicircular canal dehiscence. Am J Otolaryngol. 2026 Jan-Feb;47(1):104752. doi: 10.1016/j.amjoto.2025.104752. Epub 2025 Nov 30. PMID: 41391235. https://pubmed.ncbi.nlm.nih.gov/41391235/
- Carender WJ, Grzesiak M. Vestibular rehabilitation following surgical repair for Superior Canal Dehiscence Syndrome: A complicated case report. Physiother Theory Pract. 2018 Feb;34(2):146-156. doi: 10.1080/09593985.2017.1374491. Epub 2017 Sep 11. PMID: 28891720. https://pubmed.ncbi.nlm.nih.gov/28891720/
- Carey JP, Minor LB, Nager GT. Dehiscence or thinning of bone overlying the superior semicircular canal in a temporal bone survey. Arch Otolaryngol Head Neck Surg. 2000 Feb;126(2):137-47. doi: 10.1001/archotol.126.2.137. PMID: 10680863. https://pubmed.ncbi.nlm.nih.gov/10680863/
- Castellucci, Andrea; Piras, Gianluca; Brandolini, Cristina; Pirodda, Antonio; Modugno, Giovanni Carlo. The treatment of superior semicircular canal dehiscence: A review of the literature about a not completely clarified problem. Hearing, Balance and Communication 12(3):p 107-111, September 2014. | DOI: 10.3109/21695717.2014.941666 https://journals.lww.com/hbcm/abstract/2014/12030/the_treatment_of_superior_semicircular_canal.1.aspx
- Castellucci A, Piras G, Del Vecchio V, Crocetta FM, Maiolo V, Ferri GG, Ghidini A, Brandolini C. The effect of superior canal dehiscence size and location on audiometric measurements, vestibular-evoked myogenic potentials and video-head impulse testing. Eur Arch Otorhinolaryngol. 2021 Apr;278(4):997-1015. doi: 10.1007/s00405-020-06169-3. Epub 2020 Jun 26. PMID: 32592013. https://pubmed.ncbi.nlm.nih.gov/32592013/
- Cloutier JF, Bélair M, Saliba I. Superior semicircular canal dehiscence: positive predictive value of high-resolution CT scanning. Eur Arch Otorhinolaryngol. 2008 Dec;265(12):1455-60. doi: 10.1007/s00405-008-0672-2. Epub 2008 Apr 16. PMID: 18415114. https://pubmed.ncbi.nlm.nih.gov/18415114/
- Dumas G, Curthoys I, Castellucci A, Dumas L, Peultier-Celli L, Armato E, Malara P, Perrin P, Schmerber S. Skull Vibration-Induced Nystagmus in Superior Semicircular Canal Dehiscence: A New Insight into Vestibular Exploration-A Review. Audiol Res. 2024 Jan 22;14(1):96-115. doi: 10.3390/audiolres14010009. PMID: 38391766; PMCID: PMC10886119. https://pubmed.ncbi.nlm.nih.gov/38391766/
- Fritz CG, Casale GG, Kana LA, Hong RS. An evidenced-based diagnostic tool for superior semicircular canal dehiscence syndrome. J Otol. 2023 Oct;18(4):230-234. doi: 10.1016/j.joto.2023.09.006. Epub 2023 Sep 20. PMID: 37877067; PMCID: PMC10593562. https://pmc.ncbi.nlm.nih.gov/articles/PMC10593562/
- Gianoli GJ. Does Superior Semicircular Canal Dehiscence Surgery Resolve or Exacerbate Positional Vertigo? Audiol Res. 2025 Nov 28;15(6):165. doi: 10.3390/audiolres15060165. PMID: 41440500; PMCID: PMC12729882. https://pmc.ncbi.nlm.nih.gov/articles/PMC12729882/
- Khalili R, Jha S, Lesinszki LS, Jiang H, Bernad PG. Bilateral Superior Semicircular Canal Dehiscence Presenting as Progressive Gait Instability in a Patient With Parkinsonism and Autoimmune Features. Cureus. 2026 Feb 10;18(2):e103368. doi: 10.7759/cureus.103368. PMID: 41835739; PMCID: PMC12981735. https://pmc.ncbi.nlm.nih.gov/articles/PMC12981735/?utm_source
- Kontorinis G, Lenarz T. Superior semicircular canal dehiscence: a narrative review. J Laryngol Otol. 2022 Apr;136(4):284-292. doi: 10.1017/S0022215121002826. Epub 2021 Oct 7. PMID: 34615564. https://pubmed.ncbi.nlm.nih.gov/34615564/
- Mekonnen M, Lum M, Duong C, Rana S, Mozaffari K, Hovis GEA, Yang I. Superior semicircular canal dehiscence postoperative outcomes: a case series of 350 repairs. Acta Neurochir (Wien). 2024 May 24;166(1):230. doi: 10.1007/s00701-024-06115-w. PMID: 38789840; PMCID: PMC11126457. https://pubmed.ncbi.nlm.nih.gov/38789840/
- Naert L, Van de Berg R, Van de Heyning P, Bisdorff A, Sharon JD, Ward BK, Van Rompaey V. Aggregating the symptoms of superior semicircular canal dehiscence syndrome. Laryngoscope. 2018 Aug;128(8):1932-1938. doi: 10.1002/lary.27062. Epub 2017 Dec 27. PMID: 29280497. https://pubmed.ncbi.nlm.nih.gov/29280497/
- Sood D, Rana L, Chauhan R, Shukla R, Nandolia K. Superior semicircular canal dehiscence: A new perspective. Eur J Radiol Open. 2017 Nov 14;4:144-146. doi: 10.1016/j.ejro.2017.10.003. PMID: 29234688; PMCID: PMC5717502. https://pubmed.ncbi.nlm.nih.gov/29234688/
- Ward BK, van de Berg R, van Rompaey V, Bisdorff A, Hullar TE, Welgampola MS, Carey JP. Superior semicircular canal dehiscence syndrome: Diagnostic criteria consensus document of the committee for the classification of vestibular disorders of the Bárány Society. J Vestib Res. 2021;31(3):131-141. doi: 10.3233/VES-200004. PMID: 33522990; PMCID: PMC9249274. https://pubmed.ncbi.nlm.nih.gov/33522990/