Vestibular schwannoma (acoustic neuroma)
What is a Vestibular Schwannoma?
Vestibular schwannoma, also called acoustic neuroma, is a benign nerve sheath tumor that develops from Schwann cells of the vestibular portion of cranial nerve VIII. This nerve carries balance and hearing information between the inner ear and brain (Goldbrunner et al., 2020; Silva et al., 2023).
Vestibular schwannomas usually arise in the internal auditory canal and may extend into the cerebellopontine angle. Most are unilateral and sporadic (Goldbrunner et al., 2020).
These tumors are often slow growing, but growth behavior varies, and some remain stable during observation (Marinelli et al., 2022; Wu et al., 2022).
History
- 1777: First documented description by Eduard Sandifort following postmortem examination.
- 1895: First successful surgical removal performed by Thomas Annandale.
- 1917: Harvey Cushing published foundational work on tumors of the auditory nerve and cerebellopontine angle.
- Late 20th century: MRI improved earlier detection and helped shift some cases toward observation.
- 1980s–1990s: Stereotactic radiosurgery became an established treatment option for selected patients.
- Modern era: Management is individualized, including observation, radiosurgery, or surgery depending on tumor and patient factors.
References: (Goldbrunner et al, 2020; Silva et al, 2023)

Dr. Eduard Sandifort

Dr. Harvey Cushing
Etiology
Vestibular schwannomas are associated with dysfunction of the NF2 tumor suppressor gene on chromosome 22, which leads to loss of normal control over Schwann cell growth. This results in slow, abnormal proliferation of Schwann cells along the vestibular nerve (Goldbrunner et al, 2020).
Most cases are sporadic, meaning the genetic changes occur within the tumor itself rather than being inherited. A smaller subset is associated with NF2-related schwannomatosis, a genetic condition in which patients are more likely to develop bilateral vestibular schwannomas at a younger age (Goldbrunner et al, 2020).
Hormonal factors have been investigated, but current evidence remains inconsistent and does not establish a clear causal role (Amaral et al, 2026).

Prevalence
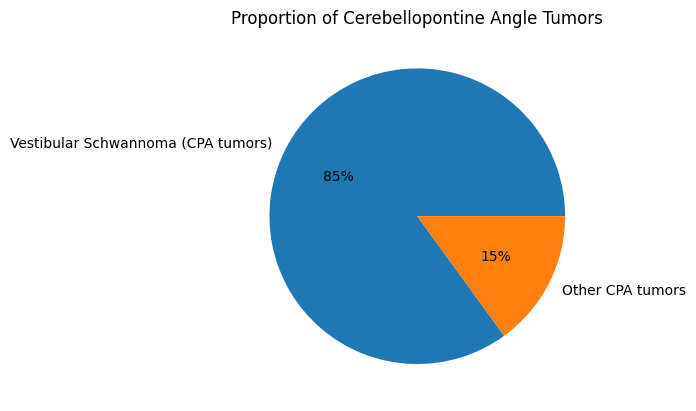
They are relatively uncommon tumors, with an estimated incidence of ~1–2 per 100,000 persons per year. They account for approximately 6–8% of all intracranial tumors and about 80–90% of tumors in the cerebellopontine angle. Increased use of MRI has led to higher detection rates, particularly of small and asymptomatic tumors identified incidentally (Goldbrunner et al, 2020; Silva et al, 2023).
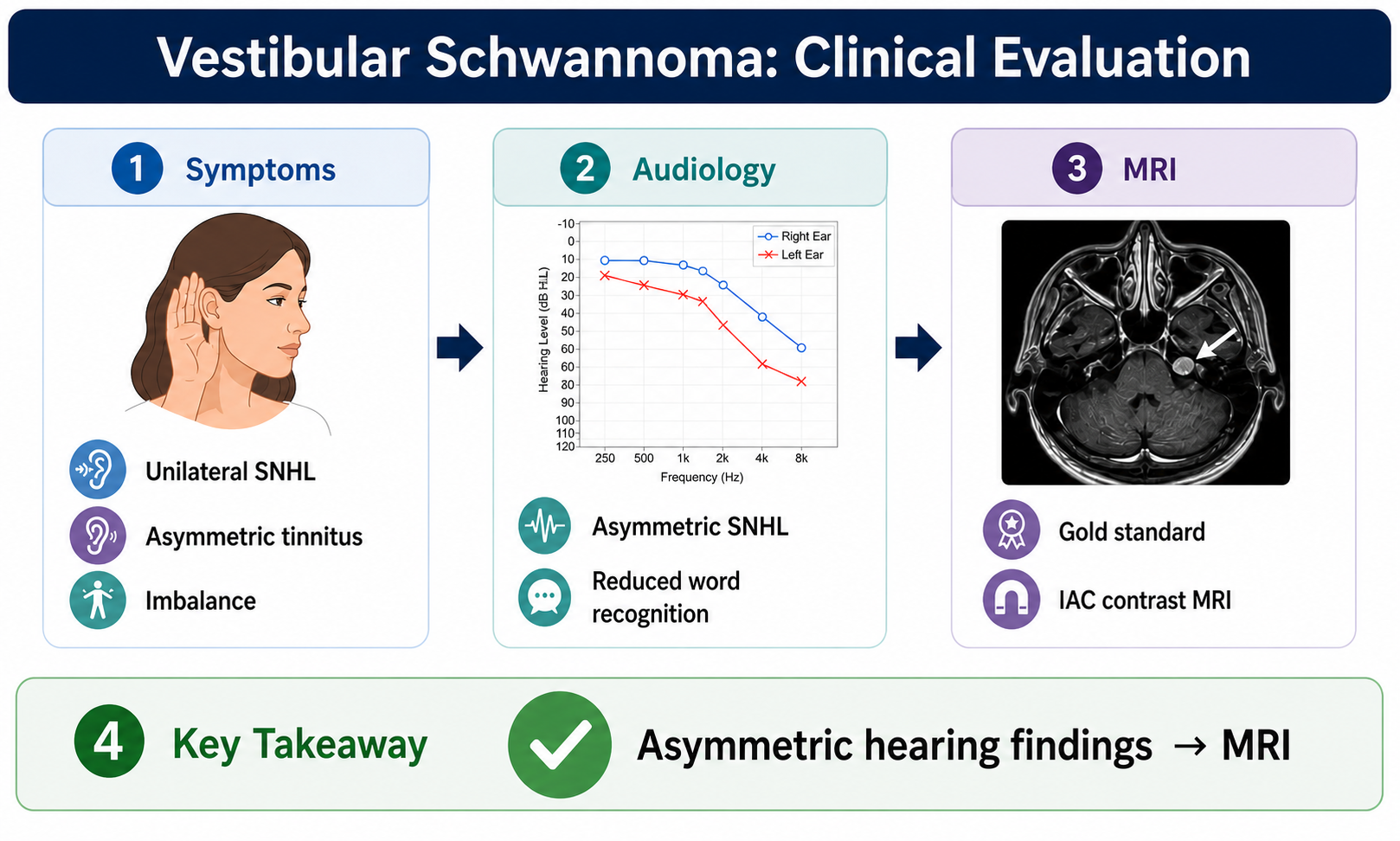
How to Diagnose Vestibular Schwannoma
Diagnosis relies on clinical suspicion, audiologic findings, and confirmatory imaging, with MRI serving as the gold standard.
- Pure tone audiometry:
- Typically demonstrates asymmetric SNHL, often high-frequency
- Speech discrimination (word recognition):
- May be disproportionately reduced relative to pure tone thresholds
- Key clinical trigger:
- Unexplained asymmetry in hearing should prompt further workup
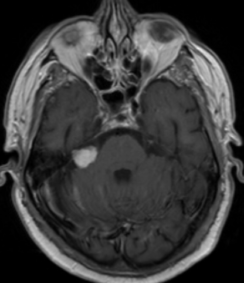
Imaging (Gold Standard)
- MRI with gadolinium contrast (IAC protocol) is the definitive diagnostic test
- Detects small intracanalicular tumors
- Defines tumor size, location (intracanalicular vs CPA), and extent
- MRI has largely replaced older screening tools due to its high sensitivity and specificity
Adjunct Testing (when MRI is unavailable or contraindicated)
- Auditory Brainstem Response (ABR):
- Can detect retrocochlear pathology
- Less sensitive for small tumors (<1 cm)
- May be used as a screening tool but does not replace MRI
Clinical Integration
Diagnosis is often initiated by audiologic asymmetry rather than vestibular findings. Importantly, dizziness alone—without hearing asymmetry—should prompt evaluation for other vestibular disorders, as vestibular schwannoma is an uncommon primary cause of vertigo (Sahyouni et al, 2017).
Key Clinical Takeaway
Any patient with unexplained asymmetric SNHL or asymmetric word recognition should be evaluated with MRI of the internal auditory canals with contrast (Goldbrunner et al, 2020; Silva et al, 2023).
Vestibular and balance findings
Supported by: Goldbrunner et al., 2020; Sahyouni et al., 2017; Silva et al., 2023
Vestibular findings in vestibular schwannoma are not diagnostic on their own, but they can help characterize functional involvement and guide rehabilitation. Patients may demonstrate findings consistent with unilateral vestibulopathy, such as reduced responses on caloric testing or reduced VOR function on vestibular testing (e.g., vHIT, head impulse test).
Spontaneous or head-shake–induced nystagmus may be present but is often low amplitude or absent due to central compensation. When present, nystagmus is typically unidirectional horizontal.
Clinically, patients more often report chronic imbalance or unsteadiness than classic episodic vertigo. When episodic vertigo is prominent, clinicians should consider coexisting vestibular disorders, such as BPPV or vestibular migraine, rather than assuming the schwannoma is the sole cause.
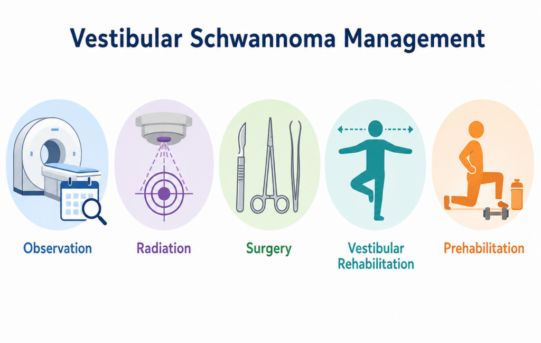
Treatment
To Learn More — Check Out These Resources
- Vestibular First’s Online, self-paced CEU courses:
- Watch related Journal Clubs:

References
- A.Hotchkies, E.Heward, A.Wadeson, et al., “Quality of Life Outcomes in Vestibular Schwannoma: A Prospective Analysis of Treatment Modalities,” The Laryngoscope135, no. 7 (2025): 2529–2537, https://doi.org/10.1002/lary.32080.
- Amaral MVGCC, Bahmad F Jr. Estrogenic/progestin therapy and the development of vestibular schwannoma: a systematic review and meta-analysis. Braz J Otorhinolaryngol. 2026;92(1):101706. https://doi.org/10.1016/j.bjorl.2025.101706
- Bambakidis, Evangeline∗; Karasik, Daniel∗,†; Mauria, Rohit∗,‡; Amin-Hanjani, Sepideh∗,‡; Mowry, Sarah E.∗,†. Barriers to Vestibular Rehabilitation in Acoustic Neuroma Surgical Patients. Otology & Neurotology 46(9):p 1158-1163, October 2025. | https://journals.lww.com/otology-neurotology/abstract/2025/10000/barriers_to_vestibular_rehabilitation_in_acoustic.31.aspx
- Breivik CN, Varughese JK, Wentzel-Larsen T, Vassbotn F, Lund-Johansen M. Conservative management of vestibular schwannoma–a prospective cohort study: treatment, symptoms, and quality of life. Neurosurgery. 2012 May;70(5):1072-80; discussion 1080. doi: 10.1227/NEU.0b013e31823f5afa. PMID: 22067416. https://pubmed.ncbi.nlm.nih.gov/22067416/
- Goldbrunner R, Weller M, Regis J, Lund-Johansen M, Stavrinou P, Reuss D, Evans DG, Lefranc F, Sallabanda K, Falini A, Axon P, Sterkers O, Fariselli L, Wick W, Tonn JC. EANO guideline on the diagnosis and treatment of vestibular schwannoma. Neuro Oncol. 2020 Jan 11;22(1):31-45. doi: 10.1093/neuonc/noz153. PMID: 31504802; PMCID: PMC6954440. https://pmc.ncbi.nlm.nih.gov/articles/PMC6954440/
- Hajikarimloo, B., Mohammadzadeh, I., Nazari, M.A. et al. Prediction of facial nerve outcomes after surgery for vestibular schwannoma using machine learning-based models: a systematic review and meta-analysis. Neurosurg Rev 48, 79 (2025). https://doi.org/10.1007/s10143-025-03230-9
- Hajikarimloo, B., Tos, S.M., Alvani, M.S. et al. Stereotactic radiosurgery for vestibular schwannomas in neurofibromatosis type 2: a systematic review and meta-analysis. BMC Cancer 25, 698 (2025). https://doi.org/10.1186/s12885-025-13959-7
- Hrubá S, Chovanec M, Čada Z, Balatková Z, Fík Z, Slabý K, Zvěřina E, Betka J, Plzak J, Čakrt O. The evaluation of vestibular compensation by vestibular rehabilitation and prehabilitation in short-term postsurgical period in patients following surgical treatment of vestibular schwannoma. Eur Arch Otorhinolaryngol. 2019 Oct;276(10):2681-2689. doi: 10.1007/s00405-019-05503-8. Epub 2019 Jun 11. PMID: 31187238. https://pubmed.ncbi.nlm.nih.gov/31187238/
- Jung GS, Montibeller GR, Fraga GS, Rohde TDS, Ramina R. Facial Nerve Adherence in Vestibular Schwannomas: Classification and Radiological Predictors. J Neurol Surg B Skull Base. 2020 Jul 1;82(4):456-460. doi: 10.1055/s-0040-1713103. PMID: 35573922; PMCID: PMC9100449. https://pmc.ncbi.nlm.nih.gov/articles/PMC9100449/
- Lees KA, Tombers NM, Link MJ, Driscoll CL, Neff BA, Van Gompel JJ, Lane JI, Lohse CM, Carlson ML. Natural History of Sporadic Vestibular Schwannoma: A Volumetric Study of Tumor Growth. Otolaryngol Head Neck Surg. 2018 Sep;159(3):535-542. doi: 10.1177/0194599818770413. Epub 2018 Apr 24. PMID: 29685084. https://pubmed.ncbi.nlm.nih.gov/29685084/
- Marinelli JP, Schnurman Z, Killeen DE, Nassiri AM, Hunter JB, Lees KA, Lohse CM, Roland JT, Golfinos JG, Kondziolka D, Link MJ, Carlson ML. Long-term natural history and patterns of sporadic vestibular schwannoma growth: A multi-institutional volumetric analysis of 952 patients. Neuro Oncol. 2022 Aug 1;24(8):1298-1306. doi: 10.1093/neuonc/noab303. PMID: 34964894; PMCID: PMC9340632. https://pubmed.ncbi.nlm.nih.gov/34964894/
- Romagna, A., Schwartz, C., Huffmann, B. et al. Analysis of quality of life and outcomes of vestibular schwannoma patients after resection and radiosurgery in an interdisciplinary treatment concept. Sci Rep 15, 15941 (2025). https://doi.org/10.1038/s41598-025-00372-0
- Sahyouni R, Moshtaghi O, Haidar YM, Mahboubi H, Moshtaghi A, Lin HW, Djalilian HR. Vertigo in Vestibular Schwannoma Patients Due to Other Pathologies. Otol Neurotol. 2017 Dec;38(10):e457-e459. doi: 10.1097/MAO.0000000000001567. PMID: 28891872; PMCID: PMC6082136. https://pubmed.ncbi.nlm.nih.gov/28891872/
- Silva VAR, Lavinsky J, Pauna HF, Vianna MF, Santos VM, Ikino CMY, Sampaio ALL, Tardim Lopes P, Lamounier P, Maranhão ASA, Soares VYR, Polanski JF, Denaro MMC, Chone CT, Bento RF, Castilho AM. Brazilian Society of Otology task force – Vestibular Schwannoma ‒ evaluation and treatment. Braz J Otorhinolaryngol. 2023 Nov-Dec;89(6):101313. doi: 10.1016/j.bjorl.2023.101313. Epub 2023 Aug 28. PMID: 37813009; PMCID: PMC10563065. https://pubmed.ncbi.nlm.nih.gov/37813009/
- Torrents Torrero A, Callejo Castillo À, Parés Martínez D, Durà Mata MJ. Preoperative interventions to improve clinical results in patients with vestibular schwannoma: A systematic review. J Vestib Res. 2026 Feb 3:9574271261420125. doi: 10.1177/09574271261420125. Epub ahead of print. PMID: 41631467. https://pubmed.ncbi.nlm.nih.gov/41631467/
- Walter J, Greene JS, Gadre AK. Vestibular Schwannoma Presenting with Cough-Induced Vertigo. J Int Adv Otol. 2023 Jan;19(1):66-69. doi: 10.5152/iao.2023.22634. PMID: 36718040; PMCID: PMC9984915. https://pmc.ncbi.nlm.nih.gov/articles/PMC9984915/
- Wu MJ, Knoll RM, Chen JX, Reinshagen K, Roychowdhury P, McKenna MJ, Kozin ED, Remenschneider AK, Jung DH. A Subset of Intracanalicular Vestibular Schwannomas Demonstrates Minimal Growth Over a 10-Year Period. Otol Neurotol. 2022 Mar 1;43(3):376-384. doi: 10.1097/MAO.0000000000003436. PMID: 35020686. https://pubmed.ncbi.nlm.nih.gov/35020686/
- Yap J, Palmer G, Graving K, Stone S, Gane EM. Vestibular Rehabilitation: Improving Symptomatic and Functional Outcomes of Persons With Vestibular Schwannoma: A Systematic Review. Phys Ther. 2024 Oct 2;104(10):pzae085. doi: 10.1093/ptj/pzae085. PMID: 38982735; PMCID: PMC11450271. https://pubmed.ncbi.nlm.nih.gov/38982735/