vestibular rehab technology for recording eye movements
When the vestibular system is faulty, abnormal eye movements (defined as nystagmus if they have slow and fast components) often result, due to the intertwining of inputs and outputs of the visual and vestibular systems. If observed by a trained researcher or clinician, the eye movements can easily differentiate between simple BPPV and more complicated conditions like concussions.
Three main technologies exist today that allow researchers and clinicians measure a patient’s eye movements with the aim of improving diagnosis and treatment:

Infrared Video Goggles
These nearly completely block room light and utilize night-vision (infrared) cameras that allow for recording of eye movements in the dark. With infrared video goggles, eye movements can be seen and recorded on a computer and enlarged for better visualization. Traditional infrared video systems are expensive, ranging from $8,500-20,000. Some require the purchase of a specific laptop and software as well as expense of training in using these components.

Frenzel Lens Goggles
This is an older technology using thickened magnifying lenses while worn in a darkened room. They are affordable at about $700 and are portable between rooms. Unfortunately, they do not provide full removal of visual fixation, and the viewing clinician must be positioned directly in front of the patient’s face in order to see the eye movements, which can be challenging with certain test and treatments. Finally, there is no way to record eye movements using Frenzel lens goggles.
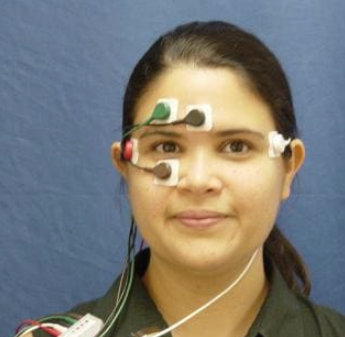
Electronystagmography (ENG)
This device was one of the first technologies developed to detect eye movements through the use of electrodes placed at specific points on the patient’s face and measuring the movements via electrical activity within the eye. Unfortunately, the setup is time-consuming and only provides data and graphs (not video recordings) of the eye. The equipment is also moderately expensive costing $5000+.
One hallmark study by Baba et al. in 2004 found that in patients with known vestibular dysfunction, 100 out of 100 demonstrated abnormal eye movements as measured by ENG, and the same 100 out of 100 demonstrated abnormal eye movements with infrared video goggles. However, only 33 out of 100 had identifiable abnormal eye movements with use of Frenzel lens goggles, indicative of their decreased ability to reduce room light. Presumably, although not included in the study, visualizing these patients’ eyes in room light (no goggles of any kind) would yield even fewer than 33 out of 100 with observable abnormal eye movements.
This makes sense because your brain tries to reduce imbalance and nausea (symptoms of vestibular dysfunction) by using visual information when in room light. Unfortunately, this also reduces or eliminates the very eye movements that a clinician can use to assist in accurate diagnosis and subsequent best treatment of vestibular conditions.
Training is also necessary to differentiate the abnormal eye movements that may result from concussion, benign paroxysmal positional vertigo (BPPV or crystals out of place in the inner ear), vestibular nerve damage, stroke, or other vestibular conditions.
However, even for experienced and trained clinicians, it is absolutely critical to be able to visualize the eye movements as accurately and fully as possible. This is particularly important if the patient may have more than one concurrent pathology present (example: known history of concussion but complains of new positional vertigo).
There are three main benefits to using infrared video goggles:
- Increased ability to visualize abnormal eye movements leading to more accurate diagnoses and appropriate treatments for patients with dizziness
- Improved confidence for vestibular therapists as they can record eye movements for later self or peer review as well as for teaching of students and mentorship of newer clinicians
- Increased profits as word of mouth and reputation as a clinic with best practice technology and improved patient outcomes result in increased patient and doctor referrals
References
- Baba S, Fukumoto A, Aoyagi M, Koizumi Y, Ikezono T, Yagi T. (2004). A Comparative Study on the Observation of Spontaneous Nystagmus with Frenzel Glasses and an Infrared CCD Camera. Journal of Nippon Medical School. 71 (1): 25-29. https://www.jstage.jst.go.jp/article/jnms/71/1/71_1_25/_pdf/-char/en
- Bakhit M, Heidarian A, Ehsani S, Delphi M, Latifi S. (2014). Clinical assessment of dizzy patients: the necessity and role of diagnostic tests. Global Journal of Health Science. 6 (3): 194-199.
- Barin K. (2007). The Fixation Suppression Test in ENG Evaluation. Audiology Online. https://www.audiologyonline.com/articles/fixation-suppression-test-in-eng-949. Accessed 12 Apr 2018.
- Blakley B, Chan L. ( 2015). Methods considerations for nystagmography. Journal of Otolaryngology, Head and Neck Surgery. 44 (25). Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4501377/
- Gananca M, Caovilla H, Gananca F. (2010). Electronystagmography versus videonystagmography. Brazilian Journal of Otorhinolaryngology (Impr.). 76 (3): 399-403. Full text: http://www.scielo.br/pdf/bjorl/v76n3/en_v76n3a21.pdf or http://www.scielo.br/scielo.php?pid=s1808-86942010000300021&script=sci_arttext&tlng=en
- Hain T. “Frenzel goggles.” Dizziness and Balance. Chicago Hearing and Balance, 3 August 2016. Web. Accessed 12 April 2018.
- Huh YE, Kim JS. (2013). Bedside evaluation of dizzy patients. Journal of Clinical Neurology. 9 (4): 203-213. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3840130/
- Klaus J, Strupp M, Siegbert K, Schuler O, Glasauer S, Brandt T. (2002). Suppression of eye movements improves balance. Brain. 125 (9): 2005-2011.
- Ruckenstein MJ, Shepard N. (2000). Balance function testing: a rational approach. Practical Issues in the Management of the Dizzy and Balance Disorder Patient. 33 (3): 507-517.
- Stern RM, Hu S, Anderson RB, Leibowitz HW, Koch KL. (1990). The effects of fixation and restricted visual field on vection-induced motion sickness. Aviation Space and Environmental Medicine. 61 (8): 712-715.
- Webb NA, Griffin MJ. (2002). Optokinetic stimuli: motion sickness, visual acuity, and eye movements. Aviation Space and Environmental Medicine. 73 (4): 351-358.
