essential equipment for a vestibular rehabilitation clinic
Whether you’re starting a vestibular rehab program on your own or joining a team of vestibular clinicians, you’ll want to make sure that you have equipment that is reliable, affordable, and works for your space. When I brought vestibular rehab to a small, previously ortho focused clinic, I compiled a list of items that I felt would be essential to a successful vestibular program. Now I’m sharing that list with you!

Keeping your equipment up to date is an important part of excellent patient care!
Basic Needs
These elements are your bare-necessities for any vestibular clinician. The items listed below include essential exam items such as infrared video goggles as well as treatment tools like make-your-own Brock strings for convergence. Think we missed something? Please email helena@vestibularfirst.com so I can share your ideas!
Most of the items below you can find on Amazon or at specialty stores linked below. If you would like to see the complete list of items from Amazon, check out our Ideas List for Essential Equipment for Vestibular Rehabilitation . Items purchased though these links directly support our innovation research to provide affordable vestibular technology to clinicians, educators, and researchers worldwide.
Post-It Notes
Post-it notes are the mainstay of the tool box for many vestibular therapists. With a clearly written, reading size letter (or larger, depending on the patient’s vision and the goals of the activity), the post-it is a solid target for active eye and head movements (also known as gaze substitution or shift) and gaze stabilization exercises (VORx1 or x2). You can have the patient hold the post-it or stick it to the wall (which is handy if they have shoulder issues or a mild tremor particularly).
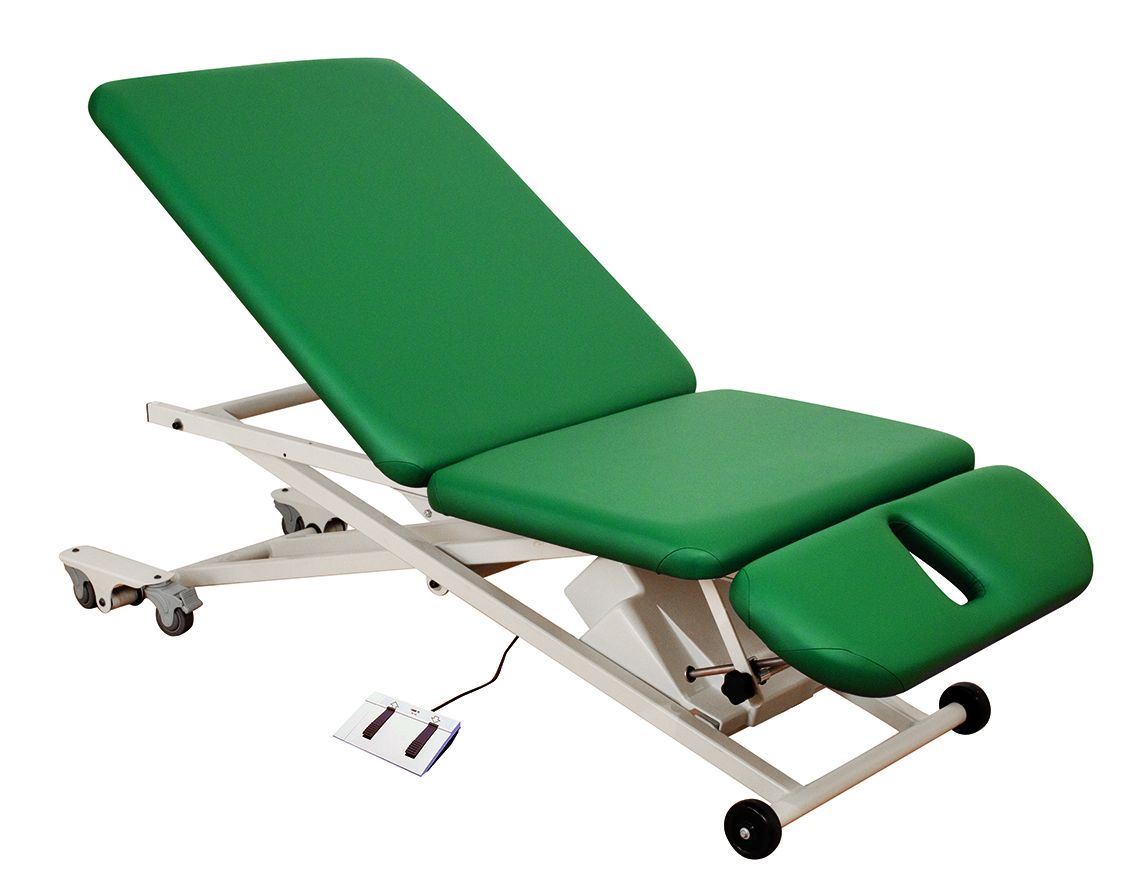
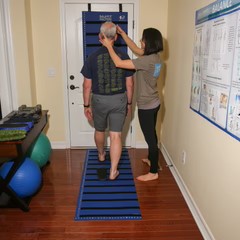
Hi Lo Lift Table
A hi lo lift table is necessary for assessment and treatment of everything from BPPV to neck issues to habituation of position changes. The adjustable height feature is important for both patient safety (getting on/off the table) as well as for proper body mechanics for the clinician. I like tables that are on the wider side, if your clinic can accommodate them, along with those that have a weight capacity to accommodate a variety of patient body types. Wider tables also allow more room for movement without the already dizzy and possibly anxious patient feeling like they might fall off of the table edge!
Rolling Stool
Your standard rolling stool will do unless you have particular ergonomic considerations for yourself or your set-up. $75 isn’t bad for a piece of equipment you will use every day for sure.
Timer
Set this timer for 30 sec, 1 min, or any time you’d like and have it countdown to ring when the patient should stop performing exercises such as active eye and head movements (gaze substitution), VORx1 or x2, and habituation or balance activities. In addition, it is has a magnetic back, stand, and hook, so there’s always a way to keep it upright and close by. At $10, it’s a low cost useful tool!
Beads for Convergence/Brock String
Using a Brock string can be important for treating those with impaired convergence (normal: 5-7 cm from the nose), which may be seen in those with post-concussive syndrome, migraine/headache, or other central vestibular disorders. At 1.2 cm, I like the size of these beads for visualization as well as the color variety in the mix. For those with a neuro program, sorting the beads also makes for a great fine motor and/or reaching activity with or without a standing balance challenge.
String for Convergence/Brock String
Instead of spending $5-10 per string, I just make my own with the above beads and this sturdy string. I like the fact I can cut the string to any size I like and give patients a string for their home exercise program. If your time for making your own strings is limited, I’ve made some strings in advance of patient care or trained staff on how to make them, so I have a stack of them waiting for me when they’re needed!
Infrared Video Goggles
If you are performing positional BPPV tests, head shake tests, or checking for spontaneous or gaze-evoked nystagmus in room light, you are likely missing abnormal eye movements you would see in the dark. Traditional Frenzel lenses have been shown to be only 33% accurate in showing displaying abnormal eye movements in those with known vestibular dysfunction.
With infrared video goggles, you have removed visual fixation and can visualize abnormal eye movements with the same accuracy as ENG (the gold standard that uses signals from electrodes on the face to track eye movements). Video goggles also allow recording of eye movements for self or peer review or student/patient education. $2,500-10,000+ depending on manufacturer and features.
BPPV Vibrating Massager
This tool is essential because it vibrates at 92 Hz, which is close to the 100 Hz needed for an effective vibration-induced nystagmus test. This test can be very useful in identifying unilateral vestibular hypofunction regardless of whether it occurred recently or remotely. Luckily, we did a Journal Club on this topic, so you can watch a recording to learn more here. I can also use it for the occasional need to add vibration to a maneuver to clear BPPV. Vibration is required if you’re going to use the maneuver that involves vibration at the mastoid of the affected side plus the BBQ (the “Kim maneuver” or modified canalith repositioning maneuver for horizontal canal) for horizontal canal cupulolithiasis. This vibrating massager is small, inexpensive, and just takes one C battery to operate (so keep extra C batteries on hand, just in case).
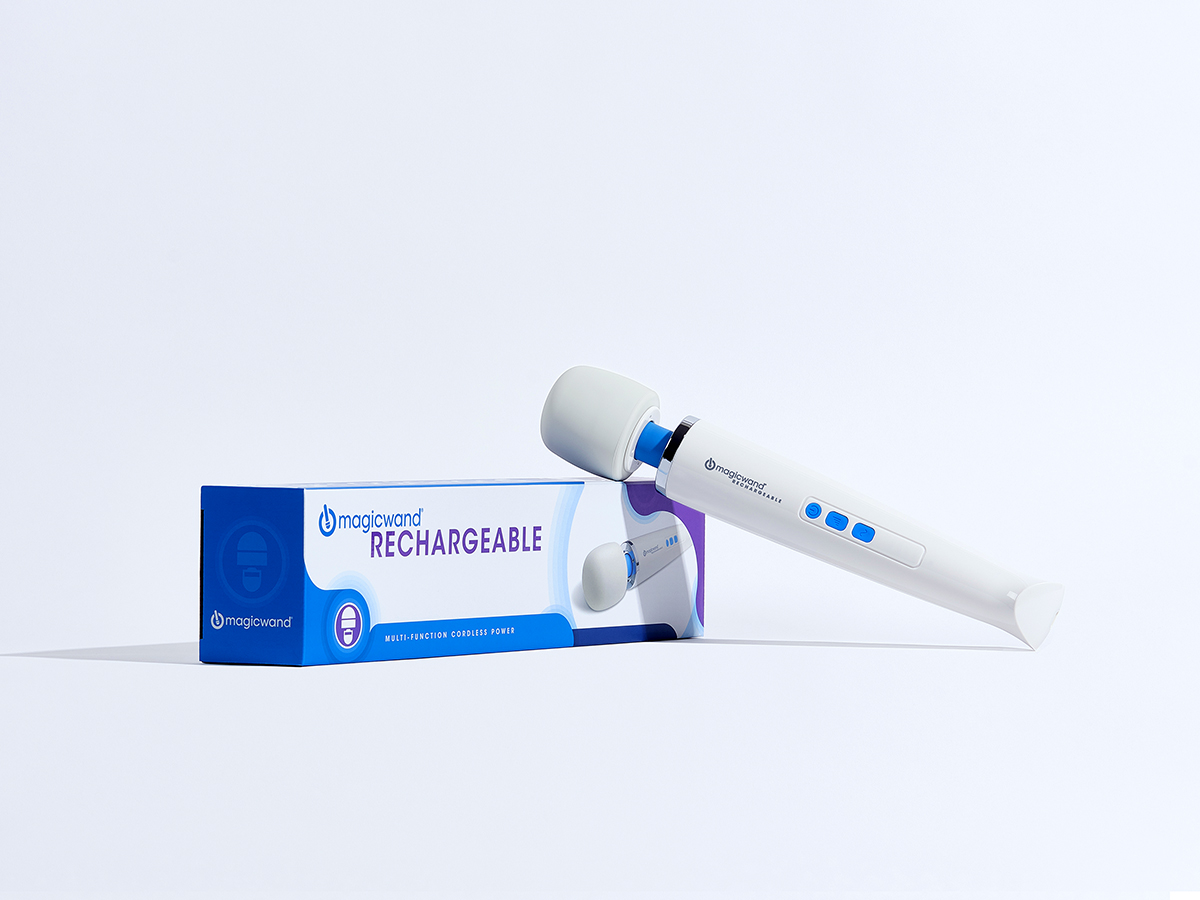
Vibration Tool
This is a more expensive vibration tool for the cordless/rechargeable version I prefer (there is a standard corded option as well). I use it sometimes for those tough BPPV cases since it has a stronger vibration that the other one I recommended. Bonus, it’s a great tool for some manual work as well (patients with vestibular issues can still have bodies with orthopedic issues, you know!).
ETDRS-R Eye Chart
Testing dynamic visual acuity is easy with this eye chart. You can choose the type you like depending on the room you have in your clinic – I prefer the one set to be accurate when the patient is standing 10 ft from the chart. You can print an eye chart for free instead of buying one, but it’s important that the patient stand at the distance appropriate for that specific chart, while it can be challenging to determine and ensure consistency of letter size between an online version and a printed one. Also, I prefer this chart because unlike a Snellen chart, there is the same number of letters on every line – in order to be counted as accurate, the patient has to read every letter on a line correctly.
Tape Measure
Every clinic likely has several tape measures floating around for assessing everything from leg length discrepancy to swelling. For a vestibular therapist, you will want to keep one handy, as you’ll need it to measure convergence, accommodation, and the distance from the rotation point of your patient’s head to a joint position error target (see more on tools for joint position error below).
Cones
This is a gold standard for a neuro or balance program, so most clinics should already have them. You can use them for cone taps to promote single limb stance balance, weaving with coordination tasks for that athletic post-concussive patient, or practicing turns for the person with vestibular loss.
Stairs or Aerobic Step
Stairs allow for assessment and treatment of an important functional task as well as serving as an element of the Functional Gait Assessment, a useful outcome measure for dynamic balance. Balance training for activities such as a step tap for single limb balance or safe negotiation when looking down may also be important for those with vestibular dysfunction. If your clinic has zero stairs available in-house and you can’t afford the space and/or cost of a wooden staircase ($900-2,000), then an aerobic step is better than nothing!
Balance Pad
A staple for any balance program, a medium density foam pad is essential for testing the mCTSIB (modified clinical test for sensory interaction in balance). It is also useful for various balance activities including stepping on/off of the foam to promote effective anticipatory and reactive control when standing or walking on uneven surfaces such as a sandy beach or a grassy yard. It won’t last forever, but it does the job well.
Joint Position Error Target
This target is free and printable for your assessment of joint position error, which if problematic may indicate possible cervicogenic dizziness. In order to be accurate, you must follow the proper protocol for target placement on the wall. This includes having the patient sit so that the rotation point of the patient’s head is 90 cm from the wall upon which you will be placing the chart, which should be eye level and centered per the patient’s report. Green and yellow are considered normal, while red and anywhere outside the target is considered abnormal.
Printable Checkerboard Pattern
Various patterned backgrounds provide an opportunity for habituation for those with visual vertigo as well as adding a level of complexity or challenge for VOR exercises or active eye/head movement (AKA gaze substitution) training. I like this checkerboard because it’s free to print, printable on standard 8.5 x 11 in paper, and easy to provide to a patient for home exercise program use as well.
360 Neuro Health Simplify Vestibular Kit
This kit includes the tools you need to perform testing for eye alignment, oculomotor, vestibular ocular reflex function, balance, motion sensitivity, and cervical kinesthetics.
Vestibular-visual-gait assessment and treatment tools are at your fingertips, plus a balance assessment protocol designed for use in concussion management programs and with higher-functioning non-concussed individuals. Another bonus: it’s fully portable for mobile PTs and outpatient clinics with multiple vestibular clinicians (although my advice is to get a kit for each clinician to avoid arm wrestling over the frequently used items). This kit is great for students and everyone from beginner to advanced clinicians because it is one of the most useful and comprehensive toolkits available. Discounts are frequently available.
Standard Shoe Boxes
To complete basic balance assessment such as an FGA or DGI, or to practice stepping over an obstacle, you will need at two standard sized shoe boxes. I bring mine in from home after buying a pair of shoes, but you can buy them online if you choose. Be warned that these will need to be replaced periodically – sometimes patients will step on them accidentally! Purchase online or get them free from a shoe store.
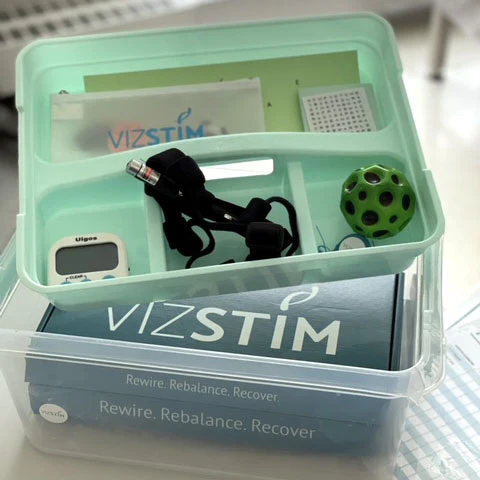
VizStim Kit
This kit is a great comprehensive starter kit for vestibular clinicians who want to make busy patient care easier and more organized for themselves. Bonus is that it includes many helpful home exercise instructions to streamline your patient education. It’s an outpatient or mobile vestibular PT’s dream come true. The VizStim Kit includes:
- VIZSTIM Concussion Kit
- VIZSTIM Vestibular Dysfunction Kit
- Timer
- Head laser
- Eye occluder
- Cervical joint position bullseye
- Brock String
- Saccades Eye Chart
- VIZSTIM Exercise Tracker PDF
- Vision Exercise Handouts
- Tote for all items
Joint Position Error Laser
This is not a significant expense if you are going to be testing joint position error for cervicogenic dizziness often. It is a very easy-to-use device and doesn’t require any fiddling with aligning the laser as it sits at midline. Its strap is thick to keep it more securely in place and comes with waist/extremity strap if you’re interested in using it for visual feedback of somatosensory positioning for other joints.
Tent Floor Sign
If your Department of Health or risk management team does not allow tape/adhesive on floors or walls, tent floor signs can be used for marking distance for balance tests such as the FGA/DGI (20 ft), gait speed/10 m walk test, or TUG. They’re customizable, easy to see, can be moved if you have limited space, and are readily cleaned. Bonus Use: Post inspirational quotes or an exercise circuit challenge of the day!
aVOR iOS App for Education
Free to download, this app provides an opportunity for patient, self, student, or new vestibular clinician education. It has a visual representation of the vestibular apparatus including its location and size relative to the head. It allows you to see which canals are activated and inhibited with certain directions of head movements as well as what types of abnormal eye movements you may see with dysfunction (acute or compensated lateral canal loss, for example). The app also has a “quiz” setting for self-testing: view the eye movements, then predict the vestibular issue(s).
Optokinetic Nystagmus Testing
To test optokinetic nystagmus (OKN) at bedside, you can use a striped material or have the patient view these scrolling lines on your screen using the OKN app. Instruct the patient to count the lines to check for appropriate optokinetic nystagmus (if absent, that’s abnormal). It’s a nice test which incorporates smooth pursuit and saccades together. On the app, clinicians can change the speed of the moving stripes, toggle the color of the stripes between Red and Black, change the width of the stripes, and reverse the direction of the stripes. Bonus: stripes can be used for a moving background for habituation in those sensitive to visual motion.
If you’d rather old-school cloth, here’s a yard of black and white striped material, or you can use a striped umbrella for torsional OKN testing.
Optokinetic Training Videos
These FREE videos are helpful for gradually progressing a habituation program for patients with visual motion sensitivity, in addition to using the disco ball (below). Three of my favorite options are:
- Gabrielle Pierce, DPT on YouTube
- Emory’s Vestibular Course Playlist
- VRT Technologies – moving lines and patterns with targets and metronome, built by Ed Kostek, PT, DPT, OCS
Adjustable Cane
Sturdy, reliable, and basic, this cane is a great tool not only for the obvious gait training but also for training stepping over an object (tree root simulation!) as long as you guard your patient closely for safety. If you have a neuro population (peripheral neuropathy etc.), you may also want to get Loftstrand crutches.
Rolling Walker
Unfortunately, vestibular issues can become so significant that a patient may need more than a cane to ensure safety while walking. This is a basic walker – if long term symptoms require ongoing use for several months or years, you can guide them through the selection of the most appropriate device (rollator with or without seat and so forth) if the basic walker does not meet their long-term needs. Consider gliders or the tried-and-true tennis balls on the back two legs of the walker, but note that the tennis balls can wear out and will need replaced if used often.
Floor Mounted Parallel Bars
Essentially, parallel are a safe place for balance training when the patient is more challenged. This includes higher level balance training, for example an athletic person on a BOSU half-dome. Your clinic’s space, the needs of your clinic (involved neuro population requires the bars to be wide enough for a wheelchair to fit in between), and your budget will likely determine which bars to purchase.
Spot It! Cards
These cards have been one of my best investments. They provide a great way to train both visual saccades (scanning to find matching objects) and left and right head turns during a balance challenge (when the cards are held by the patient with arms in a wide “V”). I have the patient reach for the cards to add another dynamic component. Not does this game make balance training less boring, but it also provides a concurrent cognitive challenge which is great for many of my patients including those with post-concussive syndrome.
Playground Ball
I like the $5 light playground balls they have at most pharmacies in the spring and summer, but if you want a sturdier ball, this one does the job. It’s great for the patient to ball toss/catch to self or to staff for anticipatory and reactive balance training. I like to walk next to my patients, alternating sides, while tossing the ball to them and having the toss it back to me, so they have to frequently turn their head while walking. It’s also perfect for the patient to toss the ball behind them, have it bounce on the wall, then they catch it, alternating sides for frequent left/right head and body turns. Increase the speed for your higher level patients, and you’ve got some significant vestibular stimulation there!
Fluid-Filled Model of Vestibular System
Showing how the otoconia move through the semicircular canals can be quite the challenge–but not anymore! Check out our new model that has crystals floating in fluid-filled canals with realistic timings, accurate anatomy, and cupulas that represent what happens during positional vertigo. $125 per apparatus ($250 for a matched left/right pair), or make your own if you want to purchase all the elements and have access to a 3D printer.
Treadmill
Although a higher priced item, a treadmill is a standard for progressing gait training, side stepping or backwards walking for a higher level patient, and completing the Balke Treadmill test. The Balke is an exertional test for patients after concussion, and it can help set heart rate limits as a patient initiates light aerobic activity with the goal of avoiding significant provocation of symptoms. I like this treadmill because it has a 15% incline (required for the Balke), but do your own research and read recent reviews, as treadmills definitely vary in quality even among the same brand/model year to year.
Recumbent Bike
Most patients need aerobic activity, particularly your patients after concussion, but they may not be safe, physically able, or tolerate the movement required on a treadmill. This is especially true with vestibular patients if they are provoked by self-motion. The recumbent bike is a great option for these patients. Again, do your own research on this one, as the brands and models seem to vary in quality year to year. I’ve had good luck with the NU step for my neuro patients (elliptical rather than circular pedal motion and can buy one with straps to secure the feet for those with a flaccid leg etc.), but they’re pricey.
Computer Stand
I like to keep my computer within easy reach for documentation, when utilizing my infrared video goggles, and to display optokinetic videos for habituation in patients with visual vertigo. Best bet is to find a computer stand that suits your space, fits your budget, and has an adjustable height.
Additional tools to consider
The below list includes bonus items that will further improve your clinic. You can save this list for months or a year or two down the road, if budget is strapped after the purchase of the essential items above.
Busy Backgrounds (e.g. wrapping paper)
If you’re ready to go beyond the checkerboard when progressing the treatment program of your patients with visual vertigo, an inexpensive way to go is wrapping paper. There are many options of varying level of challenge, from lines (vertical or horizontal depending on how you place the paper) to complex patterns. You can cover piece of cardboard for a more “permanent” use in your clinic, and you can cut off pieces for home exercise use. Another option is YouTube videos (free as long as you allow an ad to run), which can provide more challenging moving patterns, like this very difficult option: Moving Lines Video
Vestibular Today True to Life Sized Inner Ear Model
In partnership with the team at Vestibular Today, this unique and elegant model of the inner ear is printed exactly to scale. Using precious metals to highlight the beauty of this small but mighty system, it is perfect for educating patients, newer vestibular clinicians, and students on the true size of the vestibular apparatus and cochlea. Available in 18 K gold plated, sterling silver, and rose gold plated. To aid in identification, a small L or R is engraved in the cochlea to show the Left and Right ear model respectively. $75 or $150 for a matched pair.
Playing Cards
Not expensive online (maybe less at the dollar store?) but another option for reaching, picking up a flat object from the ground, cognitive training during balance activities, and tapping your toe to cards arranged in different directions on the floor for single limb balance training. My patients who like to go to the casino or play card games with friends really engage with activities involving cards. Just keep the betting out of it to avoid legal issues!
Subjective Visual Vertical App
Subjective visual vertical testing has seen a few advancements with the addition of apps to improve accuracy in testing. A great one is SaVVY, developed at the University of Alabama at Birmingham by Graham Cochrane, PhD. Unfortunately it can only be used on Android devices, so for those with Apple devices, you can consider SVV by Kuroda ENT Clinic or the Visual Vertical app. It’s a nice addition to the classic bucket test!
Proof Math Game
I found this game at the gift shop at the International Spy Museum in DC, and I couldn’t resist buying it for my patients. It can be utilized in many ways to challenge my patients’ cognitive abilities in regards to math, providing visual stimulus and encouraging frequent saccades and head turns. I will warn you, however, that some patients DO NOT love to do math problems!
Clock Yourself
Designed by an Australian physio, Clock Yourself is a great tool for adding gaming and creativity to your balance training options. It trains reactive stepping strategies and adds cognitive challenges, both of which have been shown to be important in reducing falls. It’s well worth it! Download Clock Yourself on the Apple app store or the Google Play app store.
Heart Rate Monitoring Device (chest strap or arm band)
Monitoring heart can be critical in patients post-concussion to ensure submaximal exercise or for those patients with cardiac conditions. It’s one of many clincians’ most used tools for patients with dysautonomia, used to track autonomic system recovery. I found a nicely rated and affordable option by PowrLabs, but choices abound. Similarly, an armband can be another wearable heart rate monitor choice.
Bosu Balance Trainer
The BOSU is an industry standard for higher level balance training. This is great for athletes or your more physically able patients. I like to have patients stand on the flat side, reach or toss a ball vertically or between hands to themselves, then step to turn 90 degrees and repeat. Flip the BOSU to have them stand on the round side to crank up the challenge! And good for carryover if their local gym has one too.
Balance Disc
This is a great addition to a balance program when you’re looking to diversify your uneven surfaces. I like to have my patients stand with one foot on the Airex pad and the other on the balance disc to provide a more varied challenge, then reverse the placement, all while the patient catches and tosses a ball or plays a reaching game. This is a reasonably priced item that comes in a variety of colors too.
Memory Game
While not as versatile as the Spot It! cards, a memory game is another great way to create a cognitive challenge while having a patient perform a balance exercise such as standing tandem on foam. You can select as many or few cards as you want to use, matching the game’s length to how long you want the activity to last. You can also have the patient play alone or against you or a staff member, depending on how much challenge to memory you want to provide.
Disco Ball
Party time in therapy! This disco ball is useful for those visual vertigo patients whose symptoms are provoked by busy backgrounds or visual movement, like a patterned carpet or cars moving past them. You can have them simply view the steady pattern or moving lights, perform a balance challenge while watching, or perform gaze stabilization or active eye and head movements while viewing the background. I like this disco ball in particular because I can move it between rooms or mount it to the ceiling (your choice) and adjust the color, the type of pattern, and set it to move with the beat of music or not. At this price i’s worth forgiving the fact that you need to plug it into an outlet for power.
Exercise Sliders
Place this flat disc under one foot to promote single limb balance on the opposite leg. The patient can simply slide the other leg on the floor forward/backwards or laterally then toward midline, or you can increase the challenge by having them trace letters on the floor. Backwards alphabet or spelling out words can really increase the cognitive aspect!
Marsden Ball
Work saccades, smooth pursuit, and/or head turns functionally with a Marsden ball. A staple at many vision therapy centers, this ball with letters on it hanging from a string (use a hook on your ceiling to attach) can be a great way to work on oculomotor training, a task often paired with additional balance challenges. Great for dual tasking post-concussion or really for folks with any vestibular issue. Dual tasking for the win!
Connector Toy
These are great for tossing to a patient’s left or right for them to call out the color and tap them away, challenging their magnocellular system/peripheral vision which is often disrupted in conditions such as post-concussion. Add a balance challenge and a central visual task such as finding letters on a swinging Marsden ball, and you’ve got quite the high-level task for your athletes working on return-to-play!
Alphabet Floor Mat
I love putting a foam pad in the center of this alphabet floor mat and then having my folks work on single limb balance while tapping their other foot onto different letters to spell words (cognitive task). Alternatively, have them reach their hand to touch different letters to habituate bending over/coming up with the wonderful concurrent cognitive task. Lots of options with this tool!
Cones, Rings, and Mini-Bean Bags
Ok, it looks like all my patients do is play at this point, right? So many brightly colored toys! But I’m telling you, my patients have lots more fun using these cones, rings, and bean bags for coordination, dual tasking, and magnocellular/peripheral vision work (see connector toys above) than they would sitting and marching in place. These are wonderfully portable for the mobile PT and home health folks, too!
Gaze Stability Sticks
I’m a post-it-note-on-the-wall person myself, since I prefer patients not to have to worry about keeping their “X” from moving for gaze stabilization (VORx1) exercises. However, there are cases where it’s nice to have a tongue depressor with an “X” (or another letter, as you like) on it for your patients to use. Coming in very affordably, it’s an easy “yes” even though you’ll have to write the letter on the stick yourself.
Adjustable cuff weights
Balance and vestibular patients can need resistance for strengthening too. These highly flexible cuff weights are sometimes also helpful to provide a patient with increased proprioceptive information regarding limbs.
Nice to have for the A+ Clinic
There’s no way to be an overachiever like having this swag below. Get it now while your boss still is being nice to you!
Vestibular Today Functional Inner Ear Model
This 4 inch model fits perfectly in your hand as you use it to educate yourself or others on the basics of vestibular anatomy. At the heart of the original Functional Inner Ear model is a way to simulate how gravity affects the otoconia in the semicircular canals. There is a removable ring that you can move to the affected canal to demonstrate how repositioning maneuvers work to clear the crystals. You can purchase either ear or even better–a pair that shows all six semicircular canals. This is an excellent tool for education and demonstrating the relationship between the canals. $100 per model or $200 for a matched pair.
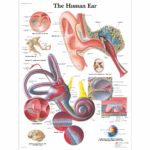
Poster of Inner Ear
A picture is worth a thousand words, and this poster is an affordable way to provide your patients with a better understanding of the vestibular system and their vestibular issues. Hang it in your office for patient education, or photocopy pictures from your vestibular textbook for the truly curious patients to take home with them as a bonus.
Tap It Game
Working on reaction time, frequent turns, and dual tasking/cognition is a breeze when using some form of light-up pods that the patient taps in response to a color and/or sound cue. I’d love to afford the highly customizable and flexible Blaze Pods or Fit Lights, but alas, at $300-1000, that is not in my current facility’s budget. So currently I use Tap It for reaction time to a certain color or as a memory game, for example.
Blink and Uno Games
Blink is great for my folks with a language barrier or moderate cognitive issues because they only have to match color, shape, or number of items on the card (no reading required). Uno is best when I want a bit more planning during game play and is especially fun if I can get a spouse or family member in on the fun. All of these games can be interspersed with physical exercise (sit to stand every time you place a card for example) and balance tasks, but the entertainment aspect tends to make them forget how long they’ve been standing/working (making fatigue less of an issue). Set the cards further apart on a table, and you get lots of frequent functional saccades/convergence and head turns. Again, dual tasking for the win!
Massage Lotion
Manual therapy is often a part of clinical care, particularly in a population that tends to have lots of cervical guarding and tightness. This massage lotion is gentle, fragrance-free, and goes on without a greasy feel. Pricing varies by amount (cheapest to buy the largest size), but I recommend getting a small amount first just to be sure you like it as much as I do!
Ping Pong Ball and Paddles
It’s fun to roll a ping pong ball back and forth to a partner or full-on play ping-pong for training in smooth pursuit, functional head and body movements, and dual tasking. Great for a super-challenge with our post-concussion athletes – standing on a BOSU ball while working to repeatedly bounce a ping pong ball on the paddle for example.
RiverStones Obstacle Balance Course
I love these river stones because they are great for walking across and around as a high level balance challenge, particularly for my patients who live downtown where negotiating curbs, cobblestone paths, and uneven sidewalks are real issues. They’ve also come in handy for outdoorsy patients who may be walking over rocky ground or into and along creeks for fishing. The real key is to cue the patients not to look down the entire time as that can be provoking to dizziness, but rather to pause while they have their balance to look ahead before looking down to continue walking.
Accommodation Ruler
For a formalized means of measuring convergence and accommodation, this ruler hits the mark. It’s pricey, which is why I keep it in my “nice to have” category. I currently measure convergence and accommodation informally with a measuring tape, which takes a bit more manual skill but is doable.
BalanceWear Vest by Motion Therapeutics
You do need to take a course to become a certified BalanceWear clinician, but it’s well worth it if you treat patients with significant vestibular loss (example: profound bilateral loss), cerebellar ataxia, or various other issues such as Multiple Sclerosis. This individualized weighted vest can be a game-changer for folks who need more somatosensory/proprioceptive input to their trunk to help significantly reduce imbalance/falls. Course cost is ~$500, and you can get a free evaluation kit if you host a course. The cost of a vest for a patient is $500-1000 depending on exact type. Often insurance can cover some or all of this cost. Even if you don’t become certified, try to find out who is in your area so you can helpfully refer patients who truly may benefit!
Activator Poles
Activator poles by Urban Poling can be a good alternative to a cane for the right patients, as they can provide improved posture, abdominal muscle activation, and larger movements for increased arm swing and stride length. They can be useful for patients with orthopedic issues such as back, hip, and knee pain as well. Clinicians can take an online webinar to learn more about how to use the Activator Poles, while there are many video resources for adults who want to use the regular urban poles for overall fitness.
Step and Connect
Step and Connect is an innovative balance and gait assessment and treatment tool. You can use the mats to assess step length and width, TUG, backward walk test, and maximal step length tests. For treatment, numerous foot shaped pads with various textures and foam densities contain clickers inside. Place the pads on the floor mat to provide visual, auditory, and tactile feedback to your patients during balance and gait training. Great for vestibular and neuro patients (I love this for my Parkinson’s patients for example). There is a home version for optimal home exercise program carryover. It’s reasonably priced for the clinic kit, or you can purchase individual elements to spread out the timing of the expenses.
Eye Occluder
I just use my hand to block the vision of one eye when testing for skew deviation. However, if you want a formalized tool, here’s an inexpensive eye occluder that can do the job. It’s affordable as well as durable and easily cleaned between patients.
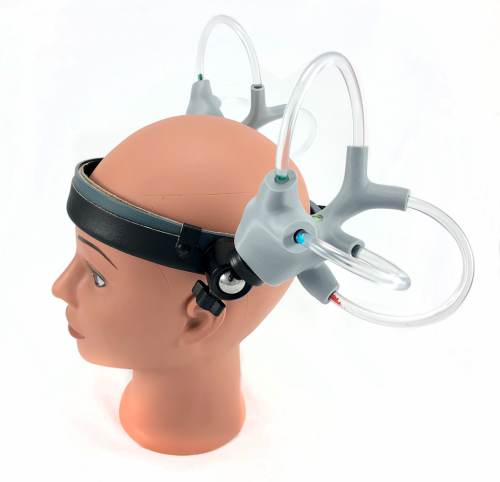
Vestibular Headband
Learn by doing with this interactive vestibular headband that shows the direct connection between the semicircular canals and the orientation of the head. We have combined the best aspects of our popular Fluid-Filled Vestibular Apparatus and attached it to an adjustable headband. Each vestibular apparatus has an embedded bubble level that helps orient the model when placed on the wearer. Awesome for vestibular educators teaching BPPV assessment and treatment at academic institutions, mentoring students and clinicians new to vestibular care, and instructing continuing ed courses. $300.
Rebounder
True confession: I don’t have one of these in my clinic. However, some clinicians swear by them as a way to increase challenge for balance, agility, and aerobic work, particularly in the athlete population. No question that bouncing can increase the stimulation to the vestibular system while challenging the core and leg muscles. Supervise patients on this closely for safety, and add multi-tasking (think math problems or single hand ball toss) for preparing for return to sport!
Shuttle Balance
Shuttle Balance is another way to introduce an unstable surface for balance training. This one provides handle bars for safety and changes the challenge depending on which direction the patient is facing (anterior/posterior vs. left/right platform sway). If you have the cash, it’s a good bonus for balance training athletes and seniors alike.