Vestibular Migraine

What is a Migraine?
“Migraine is a genetically influenced complex neurological disorder characterized by episodes of moderate-to-severe headaches, typically unilateral and frequently accompanied by nausea and heightened sensitivity to light and sound.” (Pescador Ruschel & De Jesus, 2024). These attacks can last from hours to days and may significantly interfere with daily activities.
In the most simple terms, any migraine can be understood as a “cranky brain.” This brain is hypersensitive to stimulus, puts patients in a state of abnormal sensory processing, and creates an environment where exposure to triggers can be additive until a patient crosses the “threshold” into migraine mode.
What is a Vestibular Migraine (VM)?
According to Johns Hopkins Medicine, Vestibular migraine can cause dizziness, vertigo, or imbalance with or without headache. Most patients have a history of motion sensitivity (e.g., car sickness) and have experienced migraine headaches at some point in life, even if years ago. Although not fully understood, the condition appears to stem from overlapping neural pathways that modulate pain and vestibular processing. Typical migraine triggers—such as stress, weather, hormonal changes etc.—can also precipitate vestibular migraine episodes.

History
Early 1900s –
Boenheim described migraine-related vertigo, then termed “migraine with vertigo” or “cerebral vertigo,” without defined mechanisms.
Mid–Late 1900s –
Clinicians used labels such as migrainous vertigo and migraine-associated dizziness, recognizing a migraine–vestibular link but lacking standardized criteria.
Late 1990s–2000s –
Dieterich and Brandt introduced vestibular migraine, and Neuhauser and colleagues provided epidemiologic evidence confirming it as a distinct clinical entity.
2010s–Present –
International consensus criteria established definite and probable VM, while research identified trigeminovascular and CGRP-mediated mechanisms. Recent reviews highlight VM as the most common cause of episodic vertigo with expanding therapeutic options.

Dr. Thomas Brandt

Dr. Marianne Dieterich
Etiology
VM arises from abnormal communication between the migraine pain network and central vestibular pathways. Functional and neuroanatomical studies demonstrate that the trigeminal nociceptive system – which mediates migraine pain – shares direct and indirect connections with the vestibular nuclei and thalamocortical regions, allowing migraine activity to influence balance perception and motion sensitivity (Smyth et al., 2022). Neurochemical dysregulation involving serotonin, glutamate, and calcitonin gene-related peptide (CGRP) likely heightens neuronal excitability and cross-sensitization within these shared circuits (Espinosa-Sanchez et al., 2015).
Genetic predisposition and hormonal influences—particularly fluctuating estrogen levels—contribute to the higher prevalence of VM in women and may affect threshold sensitivity to migraine triggers (Villar-Martinez et al., 2024). Neuroimaging studies further support a central origin, showing disrupted connectivity among vestibular, visual, and pain-processing areas rather than pathology in the inner ear itself (Cantillo-Martínez et al., 2025).
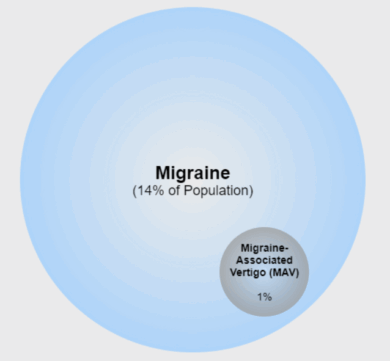
Prevalence
About 14% of the world population has migraines, and about 1% of those have Migraine-Associated Vertigo (MAV). Neuhauser et al. (2001) first estimated a lifetime prevalence of approximately 1% (1 in 100 people) and a 1-year prevalence of 0.9% in the general population, with migraine and vertigo co-occurring more often than expected by chance. More recent data from Beh (2022) suggests the prevalence may be as high as 3% when diagnostic criteria are applied. Dieterich et al. (2016) further identified VM as the most frequent cause of episodic vertigo, accounting for approximately 7% of patients in dizziness clinics and up to 9% in headache clinics, with a clear female predominance and typical onset in mid-adulthood.
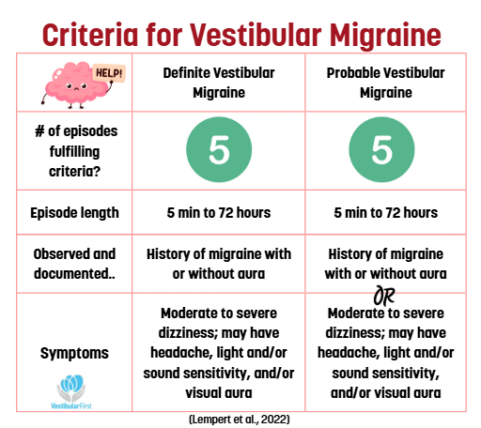
Vestibular Migraine Diagnostic Criteria – Bárány Society
A. At least five episodes fulfilling criteria C and D
B. A current or past history of 1.1 Migraine without aura or 1.2 Migraine with aura
C. Vestibular symptoms of moderate or severe intensity, lasting between 5 minutes and 72 hours
D. At least half of episodes are associated with at least one of the following three migrainous features:
- headache with at least two of the following four characteristics:
- unilateral location
- pulsating quality
- moderate or severe intensity
- aggravation by routine physical activity
- photophobia and phonophobia
- visual aura
E. Not better accounted for by another ICHD-3 diagnosis or by another vestibular disorder.
Probable Vestibular Migraine Diagnostic Criteria – Bárány Society
A. At least 5 episodes with vestibular symptoms of moderate or severe intensity, lasting 5 min to 72 hours.
B. Only one of the criteria B and C for vestibular migraine is fulfilled (migraine history or migraine features during the episode)
C. Not better accounted for by another vestibular or ICHD diagnosis
Patient Reported Symptoms
Patients with vestibular migraine typically describe recurrent attacks of vertigo or dizziness that may occur with or without headache. Vertigo can be spinning or non-spinning (rocking, tilting, swaying, or sense of motion). Attacks usually last minutes to hours, sometimes up to several days, and may be spontaneous or triggered by head motion, visual motion, or positional change.
Beh et al., 2019
Clinical Findings
Findings in vestibular migraine are highly variable — patients may show numerous abnormal results, completely normal findings, or anything in between. Between migraine episodes, central or peripheral vestibular findings may be normal or abnormal.
Possible abnormal findings include:
-
Spontaneous nystagmus, often slow and vertical
-
Abnormal saccades or impaired smooth pursuit
-
Prolonged positional nystagmus that may not match BPPV patterns or produce symptoms
In one study, Beh et al. (2019) found that 42.7% of patients (56/131) had an abnormal neuro-otologic examination between episodes, most often with:

Due to variability in clinical findings, it is essential to interpret test results alongside diagnostic criteria, patient history and symptom timing.
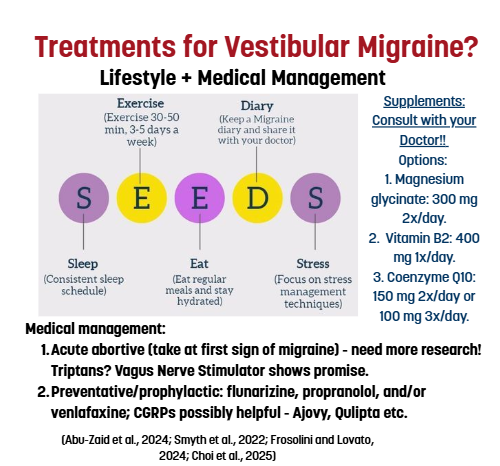
Treatment

Education
If appropriate, show patients this helpful video by Penn neurologist and migraine specialist Dr. Katherine Hamilton on when to go to the ER with a migraine and what to expect there.
Regular Exercise
Moderate-level evidence supports aerobic exercise, yoga, and structured exercise combined with lifestyle modification as effective interventions for patients with migraine—each shown to reduce headache frequency, lessen disability, and improve quality of life when performed 3–5 times per week for at least 6–8 weeks, alongside consistent sleep, nutrition, hydration, and stress-management habits (La Touche et al., 2023).
Medical Treatment
If migraines cannot be managed by avoiding triggers and regular exercise alone, some patients may need:
-
Abortive medication taken at the first sign of migraine.
-
Prophylactic medication for prevention or reduced recurrence, including new IV treatments.
-
Non-medication treatments such as vagal nerve stimulation, though more research is needed.
Refer to a neurologist or primary care physician experienced in vestibular migraine management for best results.
Sleep
Low sleep efficiency (time awake in bed vs. asleep) is linked to increased migraine frequency.
Use the Sleep Hygiene Index to assess sleep issues and make a plan to address them, including referral to a sleep specialist if needed.
Physical Therapy
Vitkovic et al. (2013) found that a 9-week guided and individualized PT program with 15 minutes of daily home exercise resulted in significant improvement, even when symptoms had been present for over a year. PT was helpful regardless of medication use.
Manual Therapy
A 2019 systematic review and meta-analysis showed that manual therapy improved quality of life in migraine patients, though data specific to vestibular migraine were not available. Several studies have also shown manual therapy to be effective in reducing cervicogenic dizziness, which can sometimes occur alongside vestibular migraine (Li and Peng, 2015; Yaseen et al., 2018; Lystad et al., 2011).
Trigger Identification
- Here are some great tips from the American Migraine Foundation on how to reduce symptoms.
- The American Headache Society provides some great resources including templates for diaries to track symptoms and possible related triggers.
- This is a comprehensive education piece by the Vestibular Disorders Association that goes into many aspects of vestibular migraine presentation and treatment.
To Learn More – Check out these Vestibular Migraine Resources
- Online, self-paced CEU course: Vestibular Migraine vs. Meniere’s Disease
- Bundle and SAVE on all courses!
- Watch related Journal Clubs:
- More Course Options
- Printable resources for patients:
- Emotional support resources for patients:
- UCLA mediation app
- Symmetry Alliance: Dr. Lisa Farrell’s page focused around vestibular migraine, PPPD
- Vestibular coaching
- The Vertigo Doctor (Dr. Madison Oak)
- The Vestibular Psychologist (Dr. Emily Kostelnik)
- The Dizzy Doctor (Dr. Paige Day)
- Learn more:
- Balancing Act Rehab: Page on Vestibular Migraine including “Talk Dizzy to Me” podcasts
References
- Ala Abu-Zaid, Sawsan Abu-Zaid, Muna Barakat, Rashed Al-Huniti, Hamzeh Khair,
Effectiveness of combination therapy of magnesium, vitamin B2 and Co-enzyme 10 supplementation on vestibular migraine: a retrospective cohort study, PHARMACIA, Volume 71, 2024, Pages 1-7,
ISSN 0428-0296. https://pharmacia.pensoft.net/article/112909/ - Beh SC, Masrour S, Smith SV, Friedman DI. The Spectrum of Vestibular Migraine: Clinical Features, Triggers, and Examination Findings. Headache. 2019 May;59(5):727-740. doi: 10.1111/head.13484. Epub 2019 Feb 8. PMID: 30737783. https://pubmed.ncbi.nlm.nih.gov/30737783/
- Beh, S.C. Vestibular Migraine. Curr Neurol Neurosci Rep 22, 601–609 (2022). https://doi.org/10.1007/s11910-022-01222-6
- Cantillo-Martínez M, Lorente-Piera J, Manrique-Huarte R, Sánchez-del-Río M, Pérez-Fernández N, Chico-Vila C, Moreno-Ajona D, Irimia P. Insights into Vestibular Migraine: Diagnostic Challenges, Differential Spectrum and Therapeutic Horizons. Journal of Clinical Medicine. 2025; 14(14):4828. https://doi.org/10.3390/jcm14144828
- Choi JH, Choi KD, Oh EH, Choi SY. Preventive medical treatment of vestibular migraine: a practical review. Res Vestib Sci. 2025;24(1):20-26. doi: 10.21790/rvs.2024.024 https://www.e-rvs.org/journal/view.php?number=990
- Dieterich M, Obermann M, Celebisoy N. Vestibular migraine: the most frequent entity of episodic vertigo. J Neurol. 2016 Apr;263 Suppl 1:S82-9. doi: 10.1007/s00415-015-7905-2. Epub 2016 Apr 15. PMID: 27083888; PMCID: PMC4833782. https://pmc.ncbi.nlm.nih.gov/articles/PMC4833782/?utm_source
- Espinosa-Sanchez JM, Lopez-Escamez JA. New insights into pathophysiology of vestibular migraine. Front Neurol. 2015 Feb 6;6:12. doi: 10.3389/fneur.2015.00012. PMID: 25705201; PMCID: PMC4319397. https://pubmed.ncbi.nlm.nih.gov/25705201/
- Frosolini A, Lovato A. Monoclonal Antibodies Targeting CGRP to Treat Vestibular Migraine: A Rapid Systematic Review and Meta-Analysis. Indian J Otolaryngol Head Neck Surg. 2024 Aug;76(4):3737-3744. doi: 10.1007/s12070-024-04578-y. Epub 2024 Mar 11. PMID: 39130214; PMCID: PMC11306672. https://pubmed.ncbi.nlm.nih.gov/39130214/
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/vestibular-migraine
- Huppert, D., Grill, E., Becker-Bense, S. et al. Diagnostic challenges in vestibular migraine—clinical differentiation from Menière’s disease and discrepancies with current classification criteria. J Neurol 272, 558 (2025). https://doi.org/10.1007/s00415-025-13291-x
- Lee YY, Yang YP, Huang PI, Li WC, Huang MC, Kao CL, Chen YJ, Chen MT. Exercise suppresses COX-2 pro-inflammatory pathway in vestibular migraine. Brain Res Bull. 2015 Jul;116:98-105. doi: 10.1016/j.brainresbull.2015.06.005. Epub 2015 Jul 4. PMID: 26151770. https://pubmed.ncbi.nlm.nih.gov/26151770/
- La Touche R, Fierro-Marrero J, Sánchez-Ruíz I, Rodríguez de Rivera-Romero B, Cabrera-López CD, Lerma-Lara S, Requejo-Salinas N, de Asís-Fernández F, Elizagaray-García I, Fernández-Carnero J, Matesanz-García L, Pardo-Montero J, Paris-Alemany A, Reina-Varona Á. Prescription of therapeutic exercise in migraine, an evidence-based clinical practice guideline. J Headache Pain. 2023 Jun 7;24(1):68. doi: 10.1186/s10194-023-01571-8. PMID: 37286937; PMCID: PMC10245624. https://pmc.ncbi.nlm.nih.gov/articles/PMC10245624/
- Lempert, T., Neuhauser, H. Epidemiology of vertigo, migraine and vestibular migraine. J Neurol 256, 333–338 (2009). https://doi.org/10.1007/s00415-009-0149-2
- Lempert T, Olesen J, Furman J, Waterston J, Seemungal B, Carey J, Bisdorff A, Versino M, Evers S, Kheradmand A, Newman-Toker D. Vestibular migraine: Diagnostic criteria1. J Vestib Res. 2022;32(1):1-6. doi: 10.3233/VES-201644. PMID: 34719447; PMCID: PMC9249276.
- Neuhauser H, Leopold M, von Brevern M, Arnold G, Lempert T. The interrelations of migraine, vertigo, and migrainous vertigo. Neurology. 2001 Feb 27;56(4):436-41. doi: 10.1212/wnl.56.4.436. PMID: 11222783. https://pubmed.ncbi.nlm.nih.gov/11222783/
- Odell, J., Clark, C., Hunnisett, A. et al. Manual therapy for chronic migraine: a pragmatic randomised controlled trial study protocol. Chiropr Man Therap 27, 11 (2019). https://doi.org/10.1186/s12998-019-0232-4
- Pescador Ruschel MA, De Jesus O. Migraine Headache. 2024 Jul 5. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 32809622. https://pubmed.ncbi.nlm.nih.gov/32809622/
- Sohn JH. Recent Advances in the Understanding of Vestibular Migraine. Behav Neurol. 2016;2016:1801845. doi: 10.1155/2016/1801845. Epub 2016 Oct 16. PMID: 27821976; PMCID: PMC5086357. https://pubmed.ncbi.nlm.nih.gov/27821976/
- Smyth D, Britton Z, Murdin L, Arshad Q, Kaski D. Vestibular migraine treatment: a comprehensive practical review. Brain. 2022 Nov 21;145(11):3741-3754. doi: 10.1093/brain/awac264. PMID: 35859353; PMCID: PMC9679161. https://pmc.ncbi.nlm.nih.gov/articles/PMC9679161/?utm_source
- Villar-Martinez, Maria D.a; Goadsby, Peter J.a,b. Vestibular migraine: an update. Current Opinion in Neurology 37(3):p 252-263, June 2024. | DOI: 10.1097/WCO.0000000000001257 https://journals.lww.com/co-neurology/fulltext/2024/06000/vestibular_migraine__an_update.9.aspx
- Vitkovic J, Winoto A, Rance G, Dowell R, Paine M. Vestibular rehabilitation outcomes in patients with and without vestibular migraine. J Neurol. 2013 Dec;260(12):3039-48. doi: 10.1007/s00415-013-7116-7. Epub 2013 Sep 24. PMID: 24061769. https://pubmed.ncbi.nlm.nih.gov/24061769/
- Yaseen K, Hendrick P, Ismail A, Felemban M, Alshehri MA. The effectiveness of manual therapy in treating cervicogenic dizziness: a systematic review. J Phys Ther Sci. 2018 Jan;30(1):96-102. doi: 10.1589/jpts.30.96. Epub 2018 Jan 27. PMID: 29410575; PMCID: PMC5788784. https://pmc.ncbi.nlm.nih.gov/articles/PMC5788784/?utm_source