Persistent Postural Perceptual Dizziness (PPPD)

What is PPPD?
Persistent Postural-Perceptual Dizziness (PPPD) is a chronic functional vestibular disorder characterized by persistent non-spinning dizziness, unsteadiness, or vertigo lasting three months or longer, which is worsened by upright posture, motion, or exposure to complex visual environments (Staab et al., 2017).
It is considered a learned form of dizziness in which the brain continues to process balance and motion information abnormally after an initial dizziness event (Staab et al., 2017; Staab, 2023). Neuroimaging studies, including functional MRI, show reduced activity and connectivity within vestibular cortical regions and increased connectivity between prefrontal, visual, and motor areas, indicating that patients rely less on vestibular input and more on visual and cognitive systems to maintain balance (Li et al., 2020; Indovina et al., 2021; Helmchen et al., 2024).
This shift leads to impaired sensory integration and greater visual dependence, which contribute to feelings of instability and dizziness in visually complex or busy environments (Tramontano et al., 2025). Over time, heightened anxiety and hypervigilance reinforce these maladaptive patterns, keeping the brain in a “high-alert” state for motion and spatial orientation (Madrigal et al., 2024).
History
PPPD evolved from several earlier diagnostic descriptions that reflected clinicians’ efforts to characterize chronic dizziness not explained by structural vestibular disease.
-
Mid-1980s – Phobic Postural Vertigo:
Described by Brandt and Dieterich (1986) as a functional balance disorder with postural instability, visual dependence, and anxiety despite normal vestibular testing. -
Early 2000s – Chronic Subjective Dizziness (CSD): Introduced by Staab and colleagues to describe persistent non-spinning dizziness and motion hypersensitivity following a vestibular or psychological event, emphasizing altered sensory perception rather than structural damage.
-
2010s – Persistent Postural-Perceptual Dizziness (PPPD): The Bárány Society (2017) unified phobic postural vertigo, CSD, and related syndromes under the diagnosis of PPPD, defined by diagnostic criteria.

Dr. Thomas Brandt

Dr. Marianne Dieterich
Etiology
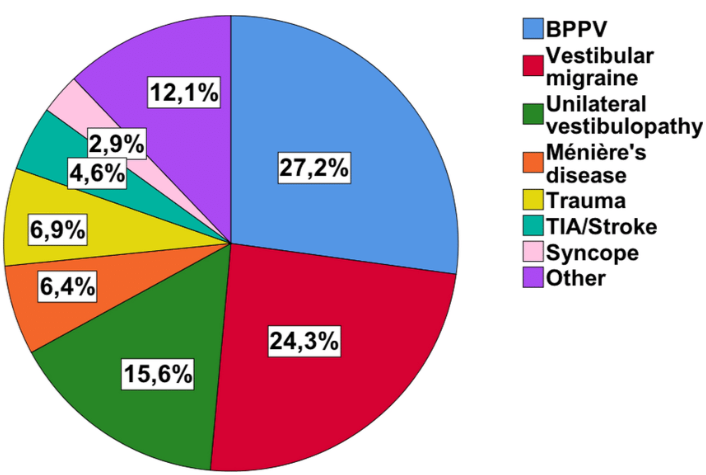
PPPD involves the onset of chronic dizziness and imbalance following an event that challenges balance, spatial orientation, or emotional stability. The disorder is typically precipitated by vestibular conditions such as benign paroxysmal positional vertigo, unilateral vestibulopathy, or vestibular migraine, but can also follow neurological illness, medical stressors, or psychological distress (Staab et al., 2017; Madrigal et al., 2024). In one case, a new onset of PPPD was observed in a patient with a history of vestibular migraine after caloric testing, reflecting an exaggerated and persistent maladaptive response to motion stimuli (Workman & Desmond, 2022).
These precipitating events lead to persistent functional alterations within the brain’s sensory and perceptual systems rather than structural injury, resulting in the sustained perception of dizziness and unsteadiness despite resolution of the initial trigger (Piatti et al., 2025; Staab, 2023).
Top Triggers for PPPD (if able to identify organic cause)
Prevalence
PPPD is the most common chronic functional vestibular disorder, accounting for approximately 15–20% of patients evaluated in tertiary dizziness or balance clinics (Staab et al., 2017; Staab, 2023; Madrigal et al., 2024). It occurs more frequently in adults between 30 and 50 years of age and shows a higher prevalence in females (Madrigal et al., 2024).
PPPD Diagnostic Criteria – Bárány Society
PPPD is a chronic vestibular disorder defined by criteria A-E below. All five criteria must be fulfilled to make the diagnosis.
A. One or more symptoms of dizziness, unsteadiness, or non-spinning vertigo are present on most days for 3 months or more.
- Symptoms last for prolonged (hours-long) periods of time, but may wax and wane in severity.
- Symptoms need not be present continuously throughout the entire day.
B. Persistent symptoms occur without specific provocation, but are exacerbated by three factors:
- Upright posture,
- Active or passive motion without regard to direction or position, and
- Exposure to moving visual stimuli or complex visual patterns.
C. The disorder is precipitated by conditions that cause vertigo, unsteadiness, dizziness, or problems with balance including acute, episodic, or chronic vestibular syndromes, other neurologic or medical illnesses, or psychological distress.
- When the precipitant is an acute or episodic condition, symptoms settle into the pattern of criterion A as the precipitant resolves, but they may occur intermittently at first, and then consolidate into a persistent course.
- When the precipitant is a chronic syndrome, symptoms may develop slowly at first and worsen gradually.
D. Symptoms cause significant distress or functional impairment.
E. Symptoms are not better accounted for by another disease or disorder.

Patient Reported Symptoms
Patients often report a persistent sensation of unsteadiness or non-spinning dizziness that is worse when upright, in motion, or exposed to visually complex environments such as crowds or scrolling screens. Symptoms often include feelings of rocking, swaying, or internal motion, rather than true vertigo, and may fluctuate in intensity throughout the day.
Many patients describe difficulty with balance, especially when walking or standing still, along with heightened sensitivity to movement, lights, or patterns. Emotional and cognitive complaints such as fatigue, concentration difficulties, and anxiety are also frequent, reflecting the disorder’s interplay between sensory processing and psychological adaptation. Importantly, hearing is typically unaffected, and the dizziness does not present as brief spinning attacks but as a continuous perception of instability lasting three months or longer (Staab et al., 2017; Popkirov et al., 2018; Staab et al., 2023).
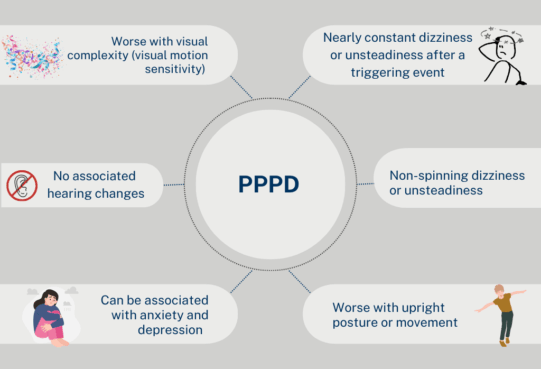
Staab et al., 2017
Clinical Findings
Often follows an acute vestibular event—most commonly BPPV or Vestibular Migraine. Clinical findings are typically subtle. Habs et al., (2020) found delayed BPPV treatment (>25 days) increases PPPD risk, especially in older adults.
-
Oculomotor exam: Typically normal
-
Dizziness: May occur during testing but typically reflects motion or visual sensitivity
-
If prior unilateral vestibulopathy: May show abnormal findings such as
-
Abnormal head impulse test
-
-
-
Vestibular testing: Usually normal or shows compensated caloric weakness; hearing typically normal.
-
Balance/Postural Control: Increased sway and dizziness on SOT (Sensory Organization Test) Conditions 3 and 6; FGA may be normal despite subjective unsteadiness.
-
Behavioral features: Visual dependence, hypervigilance, and anxiety or cognitive fatigue may be present but variable.

Treatment
Management of PPPD typically involves a multimodal approach, integrating vestibular rehabilitation therapy (VRT), psychological intervention, and pharmacologic treatment when appropriate (Staab et al., 2017; Popkirov et al., 2018). Vestibular rehabilitation therapy (VRT) plays a central role: Aims to reduce dizziness-related disability and improve balance and postural stability Targets maladaptive sensory weighting, motion sensitivity, and visual dependence Recommended as part of standard care in PPPD by expert consensus and clinical reviews (Staab et al., 2017; Popkirov et al., 2018) Psychological interventions, most commonly cognitive-behavioral therapy (CBT): Address maladaptive threat monitoring, avoidance behaviors, and symptom-focused attention Help reduce anxiety and distress that perpetuate dizziness symptoms Supported as an effective component of combined treatment approaches for PPPD (Popkirov et al., 2018; Staab, 2023) Pharmacologic treatment with SSRIs or SNRIs: Commonly used in clinical practice as an adjunct to VRT and psychological therapy May help reduce symptom severity and improve functional tolerance, particularly in patients with prominent anxiety or hypervigilance Best viewed as part of a combined treatment strategy rather than a stand-alone therapy, given limitations in controlled trial evidence (Staab et al., 2017; Staab, 2023)




To Learn More — Check Out These PPPD Resources
- Online, self-paced CEU course:
- Watch related Journal Clubs:
- More Course Options:
-
A Practical Workshop on Persistent Postural and Perceptual Dizziness presented by Janene Holmberg PT, DPT, NCS: 2 hour on demand recorded webinar
- Medbridge’s Bilateral Vestibular Disorders and PPPD online course presented by Jeff Walter
-
- Emotional support resources for patients:
- UCLA mediation app
- Symmetry Alliance: Dr. Lisa Farrell’s page focused around vestibular migraine, PPPD
- Vestibular coaching
- The Vertigo Doctor (Dr. Madison Oak)
- The Vestibular Psychologist (Dr. Emily Kostelnik)
- The Dizzy Doctor (Dr. Paige Day)
- Learn more:
- Balancing Act Rehab: Page on PPPD including podcasts
References
- Brandt T, Huppert D, Dieterich M. Phobic postural vertigo: a first follow-up. J Neurol. 1994 Feb;241(4):191-5. doi: 10.1007/BF00863767. PMID: 8195816. https://pubmed.ncbi.nlm.nih.gov/8195816/
- Habs M, Strobl R, Grill E, Dieterich M, Becker-Bense S. Primary or secondary chronic functional dizziness: does it make a difference? A DizzyReg study in 356 patients. J Neurol. 2020 Dec;267(Suppl 1):212-222. doi: 10.1007/s00415-020-10150-9. Epub 2020 Aug 27. PMID: 32852579; PMCID: PMC7718176. https://pmc.ncbi.nlm.nih.gov/articles/PMC7718176/
- Helmchen, C., Blüm, SK., Storm, R. et al. Postural motion perception during vestibular stimulation depends on the motion perception threshold in persistent postural-perceptual dizziness. J Neurol 271, 4909–4924 (2024). https://doi.org/10.1007/s00415-024-12415-z
- Indovina I, Passamonti L, Mucci V, Chiarella G, Lacquaniti F, Staab JP. Brain Correlates of Persistent Postural-Perceptual Dizziness: A Review of Neuroimaging Studies. J Clin Med. 2021 Sep 21;10(18):4274. doi: 10.3390/jcm10184274. PMID: 34575385; PMCID: PMC8468644. https://pubmed.ncbi.nlm.nih.gov/34575385/
- Li K, Si L, Cui B, Ling X, Shen B, Yang X. Altered intra- and inter-network functional connectivity in patients with persistent postural-perceptual dizziness. Neuroimage Clin. 2020;26:102216. doi: 10.1016/j.nicl.2020.102216. Epub 2020 Feb 18. PMID: 32097864; PMCID: PMC7037590. https://pubmed.ncbi.nlm.nih.gov/32097864/
- Madrigal J, Herrón-Arango AF, Bedoya MJ, Cordero Chen J, Castillo-Bustamante M. Persistent Challenges: A Comprehensive Review of Persistent Postural-Perceptual Dizziness, Controversies, and Clinical Complexities. Cureus. 2024 May 23;16(5):e60911. doi: 10.7759/cureus.60911. PMID: 38910644; PMCID: PMC11193666. https://pubmed.ncbi.nlm.nih.gov/38910644/
- Piatti D, De Angelis S, Paolocci G, Minnetti A, Manzari L, Verdecchia DH, Indovina I, Tramontano M. The Role of Vestibular Physical Therapy in Managing Persistent Postural-Perceptual Dizziness: A Systematic Review and Meta-Analysis. Journal of Clinical Medicine. 2025; 14(15):5524. https://doi.org/10.3390/jcm14155524
- Ruckenstein MJ, Staab JP. Chronic subjective dizziness. Otolaryngol Clin North Am. 2009 Feb;42(1):71-7, ix. doi: 10.1016/j.otc.2008.09.011. PMID: 19134491. https://pubmed.ncbi.nlm.nih.gov/19134491/
- Staab JP, Eckhardt-Henn A, Horii A, Jacob R, Strupp M, Brandt T, Bronstein A. Diagnostic criteria for persistent postural-perceptual dizziness (PPPD): Consensus document of the committee for the Classification of Vestibular Disorders of the Bárány Society. J Vestib Res. 2017;27(4):191-208. doi: 10.3233/VES-170622. PMID: 29036855; PMCID: PMC9249299. https://pmc.ncbi.nlm.nih.gov/articles/PMC9249299/
- Staab JP. Persistent Postural-Perceptual Dizziness: Review and Update on Key Mechanisms of the Most Common Functional Neuro-otologic Disorder. Neurol Clin. 2023 Nov;41(4):647-664. doi: 10.1016/j.ncl.2023.04.003. Epub 2023 Jun 1. PMID: 37775196. https://pubmed.ncbi.nlm.nih.gov/37775196/
- Tramontano M, Paolocci G, Piatti D, Attanasio G, Casagrande Conti L, Bergamini E, Manzari L, Lacquaniti F, Staab JP, Bosco G, Indovina I. Dynamic postural stability, symmetry, and smoothness of gait in patients with persistent postural-perceptual dizziness. J Vestib Res. 2025 Mar;35(2):82-90. doi: 10.1177/09574271241295615. Epub 2024 Nov 6. PMID: 39973598. https://pubmed.ncbi.nlm.nih.gov/39973598/
- Workman BS, Desmond AL. Persistent Postural Perceptual Dizziness Induced by Caloric Testing: A Case Report. J Am Acad Audiol. 2022 Oct;33(9-10):474-477. doi: 10.1055/a-1957-8398. Epub 2022 Oct 10. PMID: 36216343. https://pubmed.ncbi.nlm.nih.gov/36216343/
- Yagi C, Kimura A, Kai R, Yamagishi T, Ohshima S, Izumi S, Horii A. Long-term outcomes of pharmacotherapy in patients with persistent postural-perceptual dizziness. Front Neurol. 2025 Mar 19;16:1566898. doi: 10.3389/fneur.2025.1566898. PMID: 40177407; PMCID: PMC11961416. https://pubmed.ncbi.nlm.nih.gov/40177407/
- Zhang, L., Jiang, W., Tang, L. et al. Older patients with persistent postural-perceptual dizziness exhibit fewer emotional disorders and lower vertigo scores. Sci Rep 12, 11908 (2022). https://doi.org/10.1038/s41598-022-15987-w
