reducing bppv recurrence
What is BPPV (Benign Paroxysmal Positional Vertigo)?
Benign Paroxysmal Positional Vertigo, also known as BPPV, accounts for 20-30% of vestibular complaints (Sreenivas et al., 2021). BPPV occurs in the semicircular canals of the vestibular or balance sensor of a person’s inner ear. In this condition, free-floating otoconia move in one of the semicircular canals (canalithiasis) or adhere to the cupula, which is the membrane located at one end of each semicircular canal (cupulolithiasis).
What are the BPPV Basics?
The main symptoms of BPPV include recurrent brief and sudden episodes of positional vertigo when the person moves their head and body, which can assist in diagnosis even using a brief questionnaire (Kim et al, 2020). In fact, in one study of older adults by Lindell et al. in 2021, “Dizziness when turning in bed increased the risk of BPPV 8-fold.” Standard of care treatment for BPPV involves moving the otoconia back into the utricle via positional maneuvers as per the clinical practice guidelines (Bhattacharyya et al., 2017).
Why Treat BPPV?
Why don’t we just wait for it to resolve spontaneously? Only 18% of BPPV resolves spontaneously in the first month, while only 51% resolves spontaneously in a year (Álvarez-Morujo de Sande et al., 2019), leaving the rest of the patients with symptoms that interrupt life and increase risk for falls.
How often does BPPV recur?
And what about when BPPV recurs in about 27% of patients, 50% of the time within 6 months of initial episode (Perez et al., 2012)? There is a long-term recurrence rate of 13-68% in > or = 2 years (Sfakianaki et al., 2021). When otoconia debris repeatedly and unexpectedly finds its way into a person’s semi-circular canal, this can result in decreased quality of life and increased depression (Molnar et al., 2022), increasing their risk for falls and fracture (Hawke et al., 2021; Lawson et al., 2008; Liao et al., 2015), and interrupting work and daily responsibilities such as laundry or caring for a grandchild (Filippo 2017; Benecke et al., 2013; Cohen et al., 2010). Is there anything that can be done to reduce recurrence? Read on to learn more!
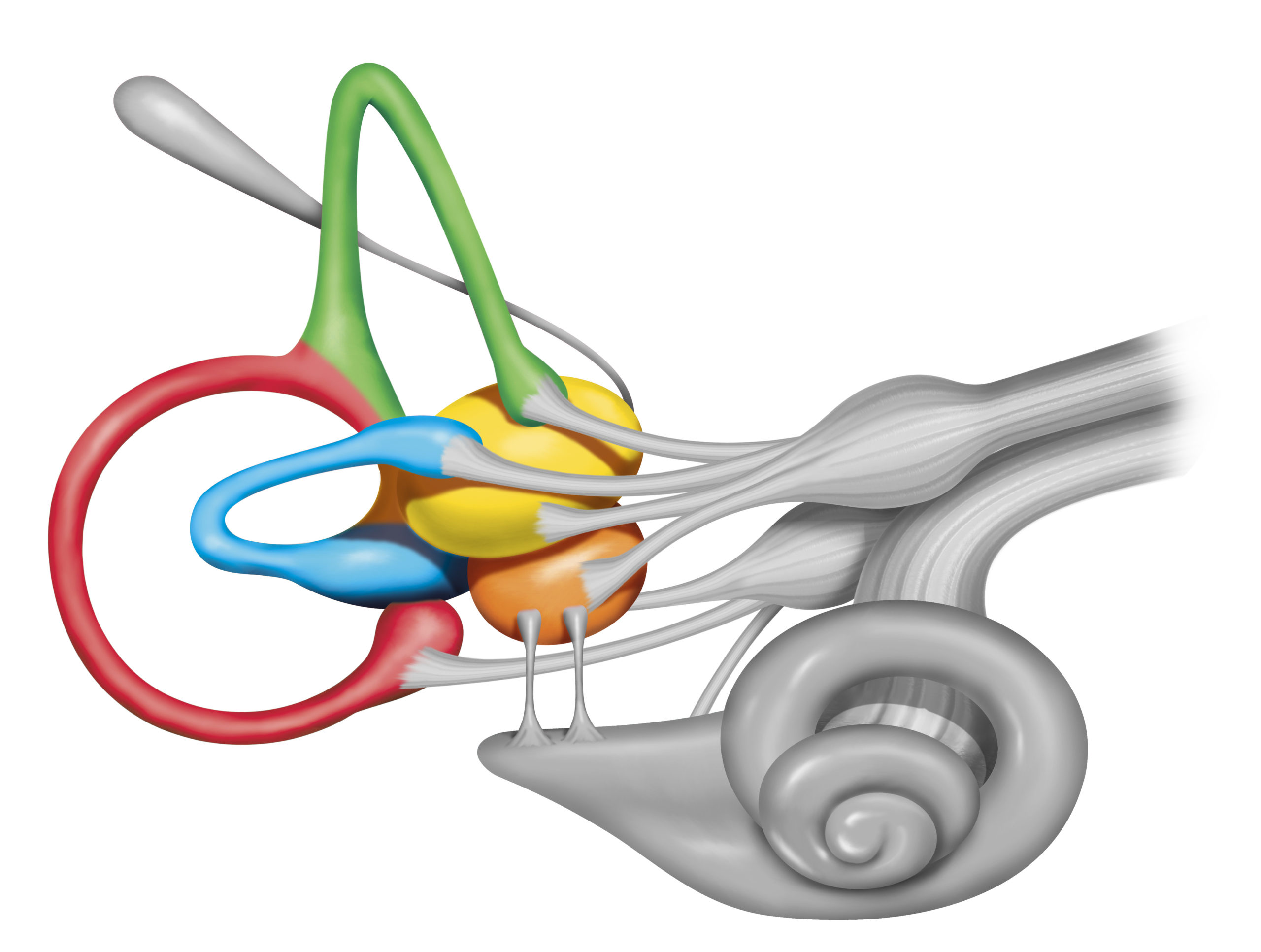
Top 2 Reasons Why BPPV Recurs AND What We Can Do About It!
- Potentially modifiable medical history risk factors – Hypertension, diabetes mellitus, hyperlipidemia, cardiovascular disease or stroke, reduced vertebral artery blood flow, osteoporosis or osteopenia, sleep disorders, and vitamin D deficiency are all known risk factors for increased recurrence of BPPV (Chen et al., 2021; Sfakianaki et al., 2021; Neri et al., 2021). Patients should work with their doctors on medical management of those conditions. For example, physicians can check a patient’s serum vitamin D level to make sure it is within normal limits. As long as not otherwise contraindicated medically, research has found that supplementation of Vitamin D 400 IU and 500 mg of calcium carbonate twice a day can reduce BPPV recurrence (Jeong et al., 2020; Jeong et al., 2022 – thanks to Dr. Sue Whitney for providing these reference details for this newsletter). This is especially important in the winter, when serum Vitamin D and physical activity levels may be lower (Meghji et al., 2017; Jiang et al, 2021). Almost all of the modifiable risk factors listed can benefit from regular physical exercise, so we can always recommend and guide safe, frequent physical activity (which is good for the patient even if they don’t have recurrent BPPV!).
- Demographic and comorbid risk factors – Age (particularly >60 years old), disruption to the peripheral vestibular structures due to conditions such as vestibular neuritis, superior semi-circular canal dehiscence, or Meniere’s disease, female gender, trauma including concussion or brain injury, migraine, bilateral/multi-canal BPPV, and cervical osteoarthrosis are all additional risk factors for BPPV (Chen et al., 2019; Barber et al., 2016; Perez et al., 2012). In addition, research has shown that a gene variant may be involved in causing or aggravating some familial cases of recurrent idiopathic BPPV (Xu et al., 2021). Patients with these factors which may influence BPPV recurrence can be educated and encouraged to address any modifiable risk factors. We can also reassure patients that there are still people with none of those risk factors who get recurrence, so we just work on what we can manage and emphasize the importance of prompt treatment when BPPV does recur.
3 Easy Strategies to Improve Posterior Canal BPPV Clearance Success!
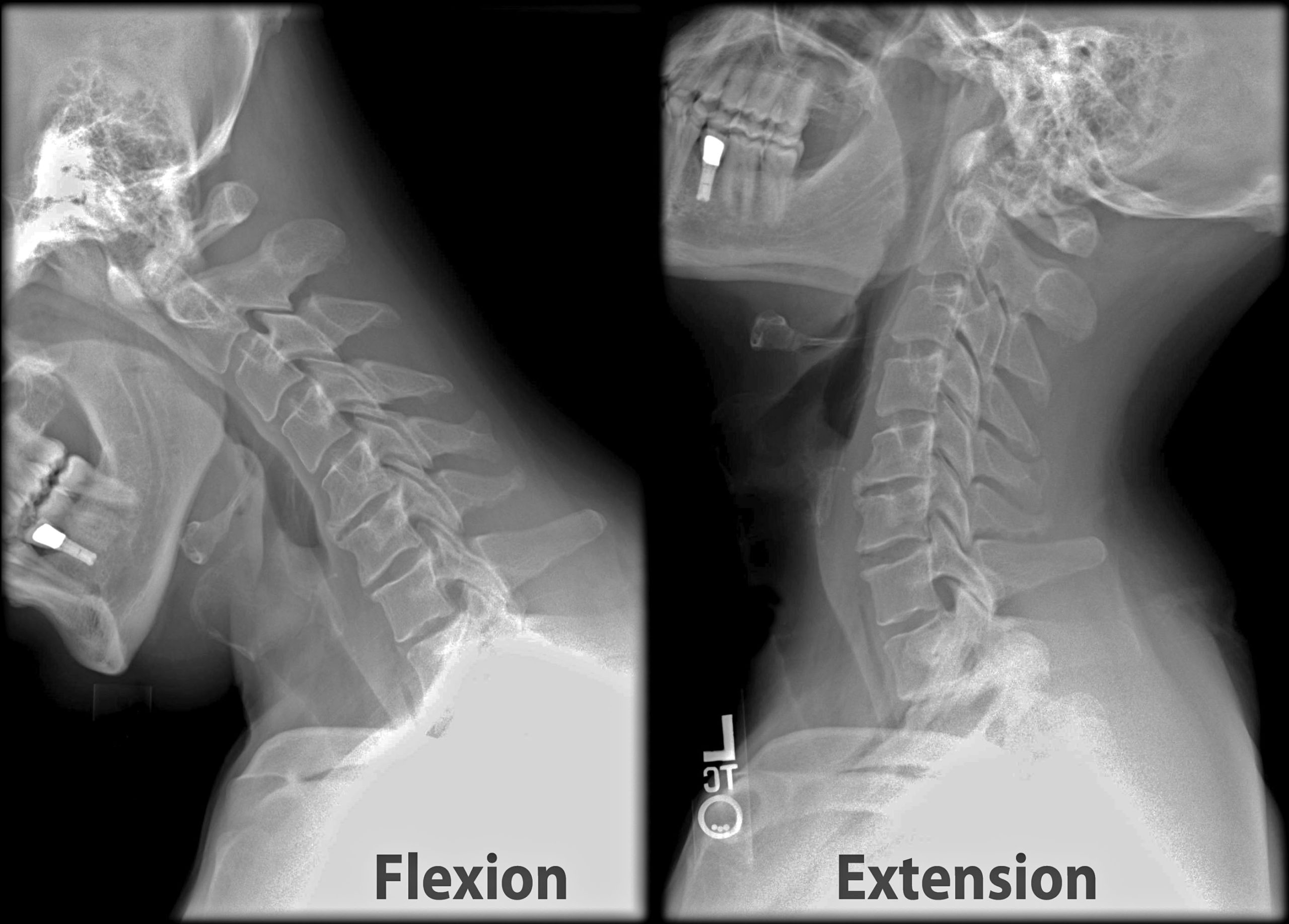
- Improve neck range of motion as much as possible! Here’s why:
According to Martellucci et al. (2019), patients with posterior canal BPPV who needed two or more canalith repositioning procedures (CRP, or modified Epley maneuvers) showed lower cervical range of motion in extension and flexion and earlier recurrences. In addition, lower cervical extension was significantly associated with the failure of the first CRP.In other words, improving cervical extension and flexion has the potential to reduce the number of maneuvers needed to clear BPPV AND may decrease recurrence! - Back-up plan “in the moment”: Modify your treatments if necessary to reduce the demand on cervical neck flexion and extension for someone with cervical range of motion limitations. Options include utilizing a tilt table (to mimic extension/flexion by positioning the body to get the head at desired angles) or utilizing maneuvers with less neck extension such as the Semont-Liberatory or if possible the Semont Plus, Gans, or the newer Li maneuver. For the Li maneuver, the patient keeps their head in neutral and goes into side-lying on their affected side x1 minute. Then, rapidly bring them to the unaffected side (1 second) and keep them in side-lying x4 minutes before sitting up with the head still in neutral to finish the maneuver.
- For stubborn posterior canal BPPV cases or when a patient cannot return as frequently for care, consider giving a repositioning maneuver to be done for a day or two at home to “seal the deal.” Lee et al. (2021) found that compared with CRP alone, combination of CRP and supine to prolonged lateral position away from the affected side improved the therapeutic effectiveness and shortened the duration of vertigo and dizziness in patients with posterior canal BPPV. While we must try to avoid converting posterior canal BPPV to lateral canal BPPV, with proper education and guided practice it can be appropriate to give a patient a home maneuver such as a self CRP (Helminski et al., 2010). If the affected side is unclear or no other maneuver can be done safely at home, a clinician can consider giving Brandt Daroff exercises (Cetin et al., 2018) in an effort to clear posterior canal BPPV.

Don’t Miss This Free Discussion: Return to Play After Concussion Journal Club
Check out our December Concussion Journal Club with top University of Michigan researcher Steve Broglio, PhD, ATC, former Denver Broncos football player and private practice owner David Bruton, Jr., PT, DPT, and renowned neuropsychologist and Director of the Concussion Program at Midwest Orthopaedics at Rush, Elizabeth Pieroth, PsyD, ABPP, MPH. This is an expert discussion you won’t want to miss – always recorded so you can view on-demand if you can’t make the live event. While you’re at it, check out our recent brilliant Journal Club with Dr. Michael Schubert on Bow Hunter’s Syndrome Mistaken as BPPV and register for our November Journal Club on the Gait Disorientation Test with Dr. Colin Grove, recent Runner-Up for the Best Research Poster at the 2022 International Conference for Vestibular Rehabilitation!

