Epley Maneuver

Description
The Epley maneuver, also known as Modified Epley, Canalith Repositioning Procedure (CRP), Canalith Repositioning Maneuver (CRM) is a procedure designed to treat posterior canalithiasis benign paroxysmal positional vertigo (BPPV) by using gravity-guided head and body rotations to move free-floating otoconia from the long arm of the posterior canal into the utricle. The movements start with the Dix-Hallpike position on the affected side, followed by a series of 90-degree head rotations and sitting upright. The procedure is highly effective and can be performed in a clinical setting or, when appropriate, taught for home use.

Effectiveness
The Epley maneuver resolves posterior canal BPPV in ~80–90% of patients within 1–3 treatments, though recurrence occurs in ~10–30% within a year, particularly in those with risk factors such as older age, head trauma, osteoporosis, or low vitamin D. A 2023 RCT (Chen et al.) found that prolonging the healthy side-lying and final head-bowed positions to 5 minutes improved first-attempt success (85% vs 63%), achieved 100% success after two attempts, and prevented canal switching. A 2024 simulation study (Arán-Tapia et al.) identified a 105° rotation in the third position and longer hold times as improving otolith clearance. These findings suggest that tailoring angles and hold durations may further improve outcomes in select patients.
History

Dr. John Epley
Dr. John Epley, an otolaryngologist, developed the maneuver in the early 1980s based on his canalithiasis theory that free-floating otoconia in the posterior canal’s long arm cause abnormal endolymph flow and vertigo. Initially met with skepticism, his work challenged earlier explanations such as utricular disease and Harold Schuknecht’s cupulolithiasis theory from the 1960s, which did not fully account for typical nystagmus patterns.
Epley’s original method used sequential head and body rotations in the canal plane, mastoid vibration, and postural restrictions to move otoconia back into the utricle. Since his first major publication in 1992, studies have confirmed the maneuver’s high efficacy, found no added benefit from vibration, and shown postural restrictions unnecessary. Today, it is the most widely used and studied treatment for posterior canalithiasis BPPV, earning a Level A recommendation in the Clinical Practice Guideline for BPPV, with modified versions continuing to be evaluated.
Instructions
The purpose of the Epley maneuver is to treat posterior canalithiasis BPPV by using a sequence of gravity-assisted head and body movements to guide free-floating otoconia out of the posterior semicircular canal and back into the utricle.
The maneuver may also be used in some cases of posterior cupulolithiasis, but it is generally less effective; this variant often responds better to Semont/liberatory maneuvers involving more rapid position changes.
Right Ear
- Explain the procedure to the patient and obtain consent.
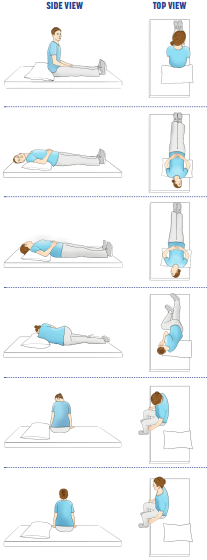
- Start seated in a long sitting position, head rotated 45° toward the right.
- Lie back quickly (if able), extending the neck over the edge of the table 20-30 deg in a Dix‑Hallpike position or extended over a pillow; hold until nystagmus stops plus ~20s.
- Rotate head 90° to the left side; hold until nystagmus stops plus ~20s.
- Roll body and head further 90° to left side-lying, face angled downward toward the mat table; hold until nystagmus stops plus ~20s.
- Return to sitting on the edge of the table, head still turned, then slowly center it. Repeat if needed.
Left Ear
- Explain the procedure to the patient and obtain consent.
- Start seated in a long sitting position, head rotated 45° toward the left.
- Lie back quickly (if able), extending the neck over the edge of the table 20-30 deg in a Dix‑Hallpike position or extended over a pillow; hold until nystagmus stops plus ~20s.
- Rotate head 90° to the right side; hold until nystagmus stops plus ~20s.
- Roll body and head further 90° to right side-lying, face angled downward toward the mat table; hold until nystagmus stops plus ~20s.
- Return to sitting on the edge of the table, head still turned, then slowly center it. Repeat if needed.
Patient Focused Handouts (PDFs)
Left ear

Related Pathology
Sources
- Arán-Tapia I, Soto-Varela A, Pérez-Muñuzuri V, Santos-Pérez S, Arán I, Muñuzuri AP. Numerical Simulations of the Epley Maneuver With Clinical Implications. Ear Hear. 2024 Jul-Aug 01;45(4):1033-1044. doi: 10.1097/AUD.0000000000001493. Epub 2024 Mar 5. PMID: 38439150; PMCID: PMC11175731. https://pubmed.ncbi.nlm.nih.gov/38439150/
- Bhattacharyya N, Gubbels SP, Schwartz SR, Edlow JA, El-Kashlan H, Fife T, Holmberg JM, Mahoney K, Hollingsworth DB, Roberts R, Seidman MD, Steiner RW, Do BT, Voelker CC, Waguespack RW, Corrigan MD. Clinical Practice Guideline: Benign Paroxysmal Positional Vertigo (Update). Otolaryngol Head Neck Surg. 2017 Mar;156(3_suppl):S1-S47. doi: 10.1177/0194599816689667. PMID: 28248609. https://pubmed.ncbi.nlm.nih.gov/28248609/
- Chen X, Mao J, Ye H, Fan L, Tong Q, Zhang H, Wu C, Yang X. The effectiveness of the modified Epley maneuver for the treatment of posterior semicircular canal benign paroxysmal positional vertigo. Front Neurol. 2023 Dec 21;14:1328896. doi: 10.3389/fneur.2023.1328896. PMID: 38187143; PMCID: PMC10771316. https://pmc.ncbi.nlm.nih.gov/articles/PMC10771316
- Epley JM. The canalith repositioning procedure: for treatment of benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg. 1992 Sep;107(3):399-404. doi: 10.1177/019459989210700310. PMID: 1408225. https://pubmed.ncbi.nlm.nih.gov/1408225/
- Hilton MP, Pinder DK. The Epley (canalith repositioning) manoeuvre for benign paroxysmal positional vertigo. Cochrane Database Syst Rev. 2014 Dec 8;2014(12):CD003162. doi: 10.1002/14651858.CD003162.pub3. PMID: 25485940; PMCID: PMC11214163. https://pubmed.ncbi.nlm.nih.gov/25485940/
- Nguyen CT, Basso M. Epley Maneuver. 2024 Sep 10. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 33085434. https://pubmed.ncbi.nlm.nih.gov/33085434/
- Sfakianaki I, Binos P, Karkos P, Dimas GG, Psillas G. Risk Factors for Recurrence of Benign Paroxysmal Positional Vertigo. A Clinical Review. J Clin Med. 2021 Sep 24;10(19):4372. doi: 10.3390/jcm10194372. PMID: 34640391; PMCID: PMC8509726. https://pubmed.ncbi.nlm.nih.gov/34640391/