Concussion

What is a Concussion?
“Concussion is a clinical syndrome of biomechanically induced alteration of brain function, typically affecting memory and orientation, which may involve loss of consciousness” (Giza et al., 2013). In simple terms, it is a type of brain injury caused by a hit, bump, or sudden movement of the head or body. This force can temporarily change how the brain works.
History
-
Early recognition (~ 1700 BCE onward) – The Edwin Smith Papyrus (ancient Egyptian medical text) described head injuries causing temporary neurological disturbance without skull fracture, and the term concussion later derived from the Latin concutere, meaning “to shake violently.”
-
Functional vs structural distinction (19th–20th century) – Physicians increasingly distinguished concussion (temporary functional brain disturbance) from contusion (structural brain injury), shaping modern mild traumatic brain injury classification.
-
Modern sport concussion standardization (2001–2002) – The First International Conference on Concussion in Sport established standardized definitions and return-to-play recommendations, initiating recurring international consensus statements.
-
Recognition of vulnerable recovery window (2012) – Experimental models showed that closely spaced concussive injuries worsen cognitive outcomes, supporting avoidance of repeat injury during early recovery (Meehan et al., 2012).
-
Evidence-based and active rehabilitation era (2013–present) – The AAN guideline formalized a modern clinical definition (Giza et al., 2013), and subsequent trials supported individualized management and early symptom-guided aerobic exercise rather than prolonged strict rest (Leddy et al., 2021; 2023).

Edwin Smith (Egyptologist)
Etiology
Concussion is a form of mild traumatic brain injury that occurs when biomechanical forces applied to the head or body cause rapid acceleration, deceleration, or rotational movement of the brain within the skull (Aubry et al., 2002; Giza et al., 2013). These forces may occur with either direct head impact or indirect forces transmitted through the body and result in a functional disturbance of brain activity rather than structural injury. Factors such as prior concussion history, injury interval, and initial symptom burden may influence outcomes (Meehan et al., 2012; Meehan et al., 2016; Chen et al., 2024).
Prevalence
Concussion is common, particularly in contact and collision sports. In the United States, an estimated 1.6 to 3.8 million sport- and recreation-related concussions occur each year, although many cases likely go unreported (Langlois et al., 2006).
In collegiate athletics, concussion incidence ranges from approximately 2 to over 30 per 10,000 athlete-exposures, with the highest rates in football and other collision sports (Wiebe et al., 2022). Outside of athletics, traumatic brain injury—including mild traumatic brain injury—occurs across the lifespan, with falls representing a major cause in older adults (Chen et al., 2024).
Diagnostic Features of Concussion
(Based on the American Academy of Neurology guideline – Giza et al., 2013)
Diagnosis is based on clinical assessment, including the history of injury and neurologic evaluation.
Common clinical features include:
-
Mechanism of injury
A direct blow to the head, face, or neck, or an impulsive force transmitted to the head from impact to the body. -
Neurologic symptoms or signs following injury
Symptoms may include headache, dizziness, confusion, memory disturbance, balance problems, or visual disturbance. -
Functional disturbance of brain activity
Concussion represents a disturbance of brain function rather than structural brain injury. -
Neuroimaging typically normal
Routine structural imaging (CT or MRI) is generally normal in concussion but may be used to evaluate for more serious injury. -
Loss of consciousness may occur but is not required.
There is no single diagnostic test or biomarker that independently confirms concussion, and diagnosis relies on clinical evaluation (Giza et al., 2013).
Patient Reported Symptoms
After a concussion, patients may report symptoms across four primary domains. Physical symptoms commonly include headache, dizziness, nausea, balance problems, and sensitivity to light or noise (Aubry et al., 2002; Giza et al., 2013). Cognitive symptoms often involve memory difficulty, slowed processing, poor concentration, or a feeling of “brain fog” (Aubry et al., 2002; Collins et al., 2014). Emotional symptoms such as irritability, anxiety, or mood changes may occur (Collins et al., 2014; Sheldrake et al., 2022), along with sleep disturbances including insomnia, increased sleep, or reduced sleep quality (Collins et al., 2014; Stevens et al., 2022). Symptoms may begin immediately or develop over the first several days and vary in intensity between individuals (Aubry et al., 2002; Giza et al., 2013).
Clinical Findings
During clinical evaluation, concussion may present with abnormalities across several neurologic and sensorimotor systems.
Neurologic Findings
A clinician may observe:
-
Disorientation or confusion
-
Slowed responses to questions
-
Impaired attention or concentration
-
Memory impairment on recall testing
-
Post-traumatic amnesia
-
Loss of consciousness (not required for diagnosis)
(Aubry et al., 2002; Giza et al., 2013; Collins et al., 2014)
Balance and Postural Control Findings
Balance testing may reveal measurable postural instability:
-
Increased sway during standing balance tests
-
Difficulty performing tandem stance or tandem gait
-
Impaired performance on standardized balance assessments
(Quatman-Yates et al., 2020; Howell et al., 2020)
Oculomotor Findings
Eye movement testing may demonstrate abnormalities in visual tracking systems:
-
Impaired smooth pursuit
-
Abnormal saccades
-
Convergence insufficiency
-
Reduced near point of convergence
(Quatman-Yates et al., 2020)
An example of a normal convergence test:
Cognitive Screening Findings
Brief cognitive testing may reveal measurable deficits:
-
Impaired immediate or delayed recall
-
Reduced attention during cognitive tasks
-
Slowed information processing
(Collins et al., 2014; Giza et al., 2013)
Cervical Spine Findings
Because concussion often occurs with rapid head and neck acceleration forces, cervical examination may reveal associated impairments:
-
Reduced cervical range of motion
-
Cervical tenderness on palpation
-
Reproduction of headache or dizziness with cervical movement
- Cervical joint position error (JPE) – assesses cervical proprioception; increased repositioning error may occur after concussion
(Kennedy et al., 2021; Smulligan et al., 2024).


Vestibular Findings
Vestibular dysfunction is common after concussion. Examination typically focuses on gaze stabilization, vestibulo-ocular reflex (VOR) function, visual motion sensitivity, and positional testing, which may indicate vestibular system involvement following head injury (Quatman-Yates et al., 2020; Collins et al., 2014).
Clinical vestibular findings may include:
-
Impaired vestibulo-ocular reflex during head-movement testing
-
Reduced dynamic visual acuity during head movement
-
Symptoms provoked with gaze stabilization or head-movement tasks
-
Visual motion sensitivity in visually complex environments
Head trauma may also dislodge otoconia within the inner ear and lead to post-traumatic benign paroxysmal positional vertigo (BPPV). Clinicians should therefore screen for BPPV. Examination may reveal:
-
Symptoms of vertigo or dizziness triggered by lying down, rolling in bed, or looking upward
-
Positional nystagmus during positional testing
Common screening tests include the Dix-Hallpike test and supine roll test (Quatman-Yates et al., 2020; Collins et al., 2014).

Treatment
Management of concussion focuses on supporting physiologic recovery and addressing the specific systems affected by the injury. Current evidence supports a brief period of relative rest followed by gradual, symptom-limited activity and targeted rehabilitation when impairments are identified (Giza et al., 2013; Quatman-Yates et al., 2020).
Early Management
During the initial 24–48 hours after injury, relative physical and cognitive rest is recommended. Activities that significantly worsen symptoms—such as intense physical exertion, prolonged screen use, or demanding cognitive tasks—should be limited. However, strict rest until symptom resolution is not recommended, as prolonged inactivity may delay recovery (Quatman-Yates et al., 2020; Leddy et al., 2023).
After the initial rest period, patients are typically encouraged to begin gradual, symptom-limited activity. Evidence from randomized controlled trials suggests that early sub-symptom threshold aerobic exercise may safely accelerate recovery compared with prolonged rest in some patients with sport-related concussion (Leddy et al., 2021).

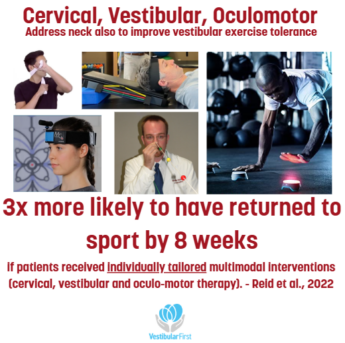
Targeted Rehabilitation
Modern concussion management emphasizes identifying the clinical domains affected by the injury and directing treatment toward those impairments. Common post-concussion clinical profiles include vestibular, oculomotor, cervical, headache/migraine, exercise intolerance, and mood-related symptoms (Collins et al., 2014; Quatman-Yates et al., 2020).
When deficits are identified, targeted rehabilitation may include:
-
Vestibular rehabilitation for dizziness, vertigo, or balance impairment
-
Oculomotor or vision therapy for abnormal eye movements or visual dysfunction
-
Cervical spine evaluation and treatment when neck injury contributes to symptoms
-
Graded aerobic exercise programs to address exertional intolerance

Management of Associated Symptoms
Patients may also require management of associated symptoms, including headache, sleep disturbance, cognitive fatigue, and emotional changes. Sleep disturbances and mental health symptoms such as anxiety or depression are commonly reported following concussion and may influence recovery (Stevens et al., 2022; Sheldrake et al., 2022).
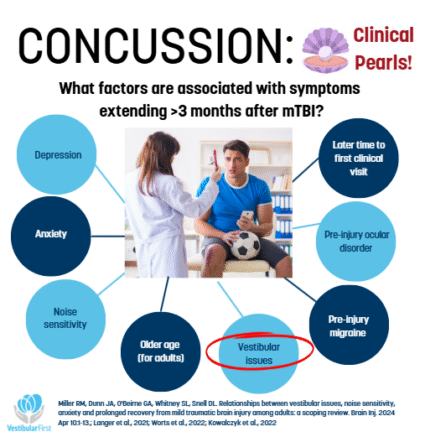
Persistent Post-Concussion Symptoms
Some individuals develop persistent post-concussion symptoms, requiring additional evaluation and treatment. Clinical guidance supports individualized, multidisciplinary rehabilitation strategies, which may include physical therapy, neuropsychology, or other specialty care depending on symptom presentation (Rytter et al., 2021).
Vestibular dysfunction and dizziness have been associated with longer recovery times in some patients, highlighting the importance of identifying and treating balance-related impairments (Miller et al., 2024).

How Long Does Concussion Recovery Take?
Recovery from a concussion can vary from person to person. Many individuals recover within the first few weeks after injury, especially with appropriate management and gradual return to activity. However, recovery time can depend on several factors, including the severity of symptoms, previous concussions, age, and overall health (Meehan et al., 2016; McIntosh et al., 2025).
Most people recover fully, but some individuals develop persistent post-concussion symptoms, where problems such as headaches, dizziness, difficulty concentrating, or fatigue last for several weeks or longer. Studies suggest that a higher number and severity of symptoms early after the injury may be associated with a longer recovery time (Meehan et al., 2016).
Certain symptoms—such as dizziness, balance problems, sleep disturbance, or emotional symptoms—may also be associated with prolonged recovery in some individuals and may require targeted rehabilitation (Miller et al., 2024; Stevens et al., 2022; Sheldrake et al., 2022).
Early evaluation and appropriate management can help identify specific problems and guide treatment to support recovery.
To Learn More – Check out these Concussion Resources
- Vestibular First’s Online, self-paced CEU course: Vestibular Examination: For Clinical Practice
- Bundle and SAVE on all courses!
- Watch related Journal Clubs:
- Treating Oculomotor Disorders after mild TBI
- BPPV After Brain Injury
-
Vestibular and the brain: Cognitive risks and benefits of dual task rehab
-
Concussion Vision Problems: Convergence, Parvocellular vs. Magnocellular Pathways, and More
- Concussion Expert Panel: Return to Play Versus Return to Academics
- Vestibular Function in Athletes with Concussion
- More Course Options
- Printable resources for patients:
- Learn more:
References
- Aubry M, Cantu R, Dvorak J, Graf-Baumann T, Johnston K, Kelly J, Lovell M, McCrory P, Meeuwisse W, Schamasch P; Concussion in Sport Group. Summary and agreement statement of the First International Conference on Concussion in Sport, Vienna 2001. Recommendations for the improvement of safety and health of athletes who may suffer concussive injuries. Br J Sports Med. 2002 Feb;36(1):6-10. doi: 10.1136/bjsm.36.1.6. PMID: 11867482; PMCID: PMC1724447. https://pubmed.ncbi.nlm.nih.gov/11867482/
- Aljabri A, Halawani A, Ashqar A, Alageely O, Alhazzani A. The Efficacy of Vestibular Rehabilitation Therapy for Mild Traumatic Brain Injury: A Systematic Review and Meta-analysis. J Head Trauma Rehabil. 2024 Mar-Apr 01;39(2):E59-E69. doi: 10.1097/HTR.0000000000000882. Epub 2024 Mar 18. PMID: 37335202. https://pubmed.ncbi.nlm.nih.gov/37335202/
- Chen Z, Wang Z, Mentis AA, Stey AM, Schwulst SJ. Factors associated with unfavorable outcomes in older patients with traumatic brain injury: analysis from the “All of Us” research program. Front Neurol. 2024 Nov 19;15:1452995. doi: 10.3389/fneur.2024.1452995. PMID: 39628897; PMCID: PMC11611856. https://pmc.ncbi.nlm.nih.gov/articles/PMC11611856/
- Chen YL, Chou TY, Sung MC, Huang YL. Sport-related Concussion Can be Prevented by Injury Prevention Program: A Systematic Review and Meta-analysis of Prospective, Controlled Studies. Sports Med Open. 2025 Nov 21;11(1):136. doi: 10.1186/s40798-025-00936-4. Erratum in: Sports Med Open. 2025 Dec 28;11(1):163. doi: 10.1186/s40798-025-00972-0. PMID: 41269468; PMCID: PMC12638499. https://pubmed.ncbi.nlm.nih.gov/41269468/
- Collins MW, Kontos AP, Reynolds E, Murawski CD, Fu FH. A comprehensive, targeted approach to the clinical care of athletes following sport-related concussion. Knee Surg Sports Traumatol Arthrosc. 2014 Feb;22(2):235-46. doi: 10.1007/s00167-013-2791-6. Epub 2013 Dec 12. PMID: 24337463. https://pubmed.ncbi.nlm.nih.gov/24337463/
- Fownes-Walpole M, Heyward O, Till K, Mackay L, Stodter A, Al-Dawoud M, Bussey MD, Gordon L, Hairsine J, Kirk C, Madden R, McBride L, McDaniel A, McKnight P, Mill N, Peek K, Pratt G, Ryan D, Salmon D, Schroeder L, Twentyman C, Versteegh T, Williams E, Jones B. Combining evidence and practice to optimise neck training aimed at reducing head acceleration events in sport: a systematic review and Delphi-consensus study. Br J Sports Med. 2025 Jul 17;59(15):1027-1042. doi: 10.1136/bjsports-2024-108847. PMID: 40345809. https://pubmed.ncbi.nlm.nih.gov/40345809/
- Gil C, Decq P. How similar are whiplash and mild traumatic brain injury? A systematic review. Neurochirurgie. 2021 May;67(3):238-243. doi: 10.1016/j.neuchi.2021.01.016. Epub 2021 Jan 30. PMID: 33529694. https://pubmed.ncbi.nlm.nih.gov/33529694/
- Giza CC, Kutcher JS, Ashwal S, Barth J, Getchius TS, Gioia GA, Gronseth GS, Guskiewicz K, Mandel S, Manley G, McKeag DB, Thurman DJ, Zafonte R. Summary of evidence-based guideline update: evaluation and management of concussion in sports [RETIRED]: report of the Guideline Development Subcommittee of the American Academy of Neurology. Neurology. 2013 Jun 11;80(24):2250-7. doi: 10.1212/WNL.0b013e31828d57dd. Epub 2013 Mar 18. PMID: 23508730; PMCID: PMC3721093. https://pmc.ncbi.nlm.nih.gov/articles/PMC3721093/
- Howell DR, Wingerson MJ, Smulligan KL, Magliato S, Simon S, Wilson JC. Exercising More Than 150 min/wk After Concussion Is Associated With Sleep Quality Improvements. J Head Trauma Rehabil. 2024 Jul-Aug 01;39(4):E216-E224. doi: 10.1097/HTR.0000000000000918. Epub 2023 Nov 6. PMID: 38032838; PMCID: PMC11070449. https://pubmed.ncbi.nlm.nih.gov/38032838/
- Howell DR, Mayer AR, Master CL, Leddy J, Zemek R, Meier TB, Owen Yeates K, Arbogast KB, Mannix R, Meehan WP 3rd. Prognosis for Persistent Post Concussion Symptoms using a Multifaceted Objective Gait and Balance Assessment Approach. Gait Posture. 2020 Jun;79:53-59. doi: 10.1016/j.gaitpost.2020.04.013. Epub 2020 Apr 20. PMID: 32361125. https://pubmed.ncbi.nlm.nih.gov/32361125/
- Kamins J, Richards R, Barney BJ, Locandro C, Pacchia CF, Charles AC, Cook LJ, Gioia G, Giza CC, Blume HK. Evaluation of Posttraumatic Headache Phenotype and Recovery Time After Youth Concussion. JAMA Netw Open. 2021 Mar 1;4(3):e211312. doi: 10.1001/jamanetworkopen.2021.1312. PMID: 33683335; PMCID: PMC7941198. https://pubmed.ncbi.nlm.nih.gov/33683335/
- Kennedy E, Chapple C, Quinn D, Tumilty S. Can the neck contribute to persistent symptoms post concussion? Long-term follow up from a prospective descriptive case series. J Man Manip Ther. 2021 Oct;29(5):318-331. doi: 10.1080/10669817.2021.1920276. Epub 2021 Jul 19. PMID: 34279185; PMCID: PMC8491693. https://pmc.ncbi.nlm.nih.gov/articles/PMC8491693/
- Langlois JA, Rutland-Brown W, Wald MM. The epidemiology and impact of traumatic brain injury: a brief overview. J Head Trauma Rehabil. 2006;21(5):375-378. https://pubmed.ncbi.nlm.nih.gov/16983222/
- Leddy JJ, Master CL, Mannix R, Wiebe DJ, Grady MF, Meehan WP, Storey EP, Vernau BT, Brown NJ, Hunt D, Mohammed F, Mallon A, Rownd K, Arbogast KB, Cunningham A, Haider MN, Mayer AR, Willer BS. Early targeted heart rate aerobic exercise versus placebo stretching for sport-related concussion in adolescents: a randomised controlled trial. Lancet Child Adolesc Health. 2021 Nov;5(11):792-799. doi: 10.1016/S2352-4642(21)00267-4. Epub 2021 Oct 1. PMID: 34600629. https://pubmed.ncbi.nlm.nih.gov/34600629/
- Leddy JJ, Burma JS, Toomey CM, Hayden A, Davis GA, Babl FE, Gagnon I, Giza CC, Kurowski BG, Silverberg ND, Willer B, Ronksley PE, Schneider KJ. Rest and exercise early after sport-related concussion: a systematic review and meta-analysis. Br J Sports Med. 2023 Jun;57(12):762-770. doi: 10.1136/bjsports-2022-106676. PMID: 37316185. https://pubmed.ncbi.nlm.nih.gov/37316185/
- Lucke-Wold B, Zasler ND, Ruchika FNU, Weisman S, Le D, Brunicardi J, Kong I, Ghumman H, Persad S, Mahan D, et al. Supplement and nutraceutical therapy in traumatic brain injury. Nutr Neurosci. 2024;28(6):709-743. doi:10.1080/1028415X.2024.2404782 https://www.researchgate.net/publication/387555056_Supplement_and_nutraceutical_therapy_in_traumatic_brain_injury
- McIntosh SJ, Vergeer MH, Galarneau JM, Eliason PH, Debert CT. Factors Associated With Persisting Symptoms After Concussion in Adults With Mild TBI: A Systematic Review and Meta-Analysis. JAMA Netw Open. 2025 Jun 2;8(6):e2516619. doi: 10.1001/jamanetworkopen.2025.16619. PMID: 40531530; PMCID: PMC12177663. https://pubmed.ncbi.nlm.nih.gov/40531530/
- Meehan WP 3rd, Zhang J, Mannix R, Whalen MJ. Increasing recovery time between injuries improves cognitive outcome after repetitive mild concussive brain injuries in mice. Neurosurgery. 2012 Oct;71(4):885-91. doi: 10.1227/NEU.0b013e318265a439. PMID: 22743360; PMCID: PMC5815628. https://pubmed.ncbi.nlm.nih.gov/22743360/
- Meehan WP 3rd, O’Brien MJ, Geminiani E, Mannix R. Initial symptom burden predicts duration of symptoms after concussion. J Sci Med Sport. 2016 Sep;19(9):722-5. doi: 10.1016/j.jsams.2015.12.002. Epub 2015 Dec 12. PMID: 26718812; PMCID: PMC4903939. https://pubmed.ncbi.nlm.nih.gov/26718812/
- Miller RM, Dunn JA, O’Beirne GA, Whitney SL, Snell DL. Relationships between vestibular issues, noise sensitivity, anxiety and prolonged recovery from mild traumatic brain injury among adults: a scoping review. Brain Inj. 2024 Jul 2;38(8):607-619. doi: 10.1080/02699052.2024.2337905. Epub 2024 Apr 10. PMID: 38597651. https://pubmed.ncbi.nlm.nih.gov/38597651/
- Reid SA, Farbenblum J, McLeod S. Do physical interventions improve outcomes following concussion: a systematic review and meta-analysis? Br J Sports Med. 2022 Mar;56(5):292-298. doi: 10.1136/bjsports-2020-103470. Epub 2021 Sep 30. PMID: 34593371. https://pubmed.ncbi.nlm.nih.gov/34593371/
- Rytter HM, Graff HJ, Henriksen HK, Aaen N, Hartvigsen J, Hoegh M, Nisted I, Næss-Schmidt ET, Pedersen LL, Schytz HW, Thastum MM, Zerlang B, Callesen HE. Nonpharmacological Treatment of Persistent Postconcussion Symptoms in Adults: A Systematic Review and Meta-analysis and Guideline Recommendation. JAMA Netw Open. 2021 Nov 1;4(11):e2132221. doi: 10.1001/jamanetworkopen.2021.32221. PMID: 34751759; PMCID: PMC8579233. https://pubmed.ncbi.nlm.nih.gov/34751759/
- Sheldrake E, Al-Hakeem H, Lam B, Goldstein BI, Wheeler AL, Burke M, Dunkley BT, Reed N, Scratch SE. Mental Health Outcomes Across the Lifespan in Individuals With Persistent Post-Concussion Symptoms: A Scoping Review. Front Neurol. 2022 Apr 11;13:850590. doi: 10.3389/fneur.2022.850590. PMID: 35481264; PMCID: PMC9035995. https://pmc.ncbi.nlm.nih.gov/articles/PMC9035995/
- Smulligan KL, Carry P, Smith AC, Esopenko C, Baugh CM, Wilson JC, Howell DR. Cervical spine proprioception and vestibular/oculomotor function: An observational study comparing young adults with and without a concussion history. Phys Ther Sport. 2024 Sep;69:33-39. doi: 10.1016/j.ptsp.2024.07.002. Epub 2024 Jul 11. PMID: 39013262; PMCID: PMC11343652. https://pubmed.ncbi.nlm.nih.gov/39013262/
- Stevens DJ, Alghwiri A, Appleton SL, Rogers JM, Plummer SL, Grant C, Bickley K, Alvaro PK, Kennett S, Adams R, Holtzhausen L. Should We Lose Sleep Over Sleep Disturbances After Sports-Related Concussion? A Scoping Review of the Literature. J Head Trauma Rehabil. 2022 May-Jun 01;37(3):E206-E219. doi: 10.1097/HTR.0000000000000701. Epub 2021 Jun 15. PMID: 34145161. https://pubmed.ncbi.nlm.nih.gov/34145161/
- Quatman-Yates CC, Hunter-Giordano A, Shimamura KK, Landel R, Alsalaheen BA, Hanke TA, McCulloch KL. Physical therapy evaluation and treatment after concussion/mild traumatic brain injury. J Orthop Sports Phys Ther. 2020;50(4):CPG1-CPG73. doi:10.2519/jospt.2020.0301. https://www.jospt.org/doi/10.2519/jospt.2020.0301
- Tinney EM, Nwakamma MC, España-Irla G, Kong L, Chen C, Hwang J, O’Brien A, Perko M, Sodemann RL, Caefer J, Manczurowsky J, Stillman A, Hillman CH, Morris TP. The feasibility and efficacy of a virtual, symptom-guided aerobic exercise intervention to improve cognition in mild traumatic brain injury: A single-blind pilot randomized control trial with an active comparator group. medRxiv [Preprint]. 2025 Dec 15:2025.12.11.25342088. doi: 10.64898/2025.12.11.25342088. PMID: 41445627; PMCID: PMC12723768. https://pmc.ncbi.nlm.nih.gov/articles/PMC12723768/
- Wiebe DJ, Bretzin AC, D’Alonzo BA; and the Ivy League–Big Ten Epidemiology of Concussion Study Investigators. Progression through return-to-sport and return-to-academics guidelines for concussion management and recovery in collegiate student athletes: findings from the Ivy League-Big Ten Epidemiology of Concussion Study. Br J Sports Med. 2022 Jul;56(14):801-811. doi: 10.1136/bjsports-2021-104451. Epub 2022 Apr 20. PMID: 35444018; PMCID: PMC9252856. https://pubmed.ncbi.nlm.nih.gov/35444018/