autoimmune vertigo top tips
What is Autoimmune Vertigo?
In autoimmune vertigo, the immune system malfunctions and attacks just the ear, the ear and some other body part like the eye, or the entire body. Damage to the inner ear structures can result in vertigo and/or hearing impairment.
Top 5 Reasons Why It’s Underdiagnosed
- First sign of disease – Vertigo and other vestibular/auditory system symptoms may be the first sign of autoimmune disease; sometimes there aren’t other autoimmune symptoms yet.
- Symptoms aren’t always present – There can be “alternating phases” of improvement related to the fluctuant nature of autoimmune disease (ex: Meniere’s Disease).
- Rare makes it less familiar – It’s easy to attribute autoimmune vertigo to more common causes e.g. “Maybe it was just BPPV”.
- There is currently no test – No test yet exists to identify inner ear specific antigens.
- Hearing loss (or lack thereof) is not diagnostic – Hearing loss may be present or not in an autoimmune vestibular condition.
Source: Girasoli et al., 2018
When should I suspect?
- Known autoimmune disease such as lupus or MS
- Fluctuant, sometimes sequential (left then right or vice versa), and frequently bilateral vertigo and/or hearing impairment symptoms, often without an identifiable trigger
- Other symptoms of autoimmune disease (example: dry eye in Sjogren’s)
- Positive blood tests for systemic autoimmune diseases – possible tests include antinucleus antibodies (ANA), serum immunoglobulins IgG, IgA, and IgM, C3 and C4 complement factors, and immunophenotype of peripheral blood lymphocytes (PBL)
- Positive response (reduction in symptoms) to steroids
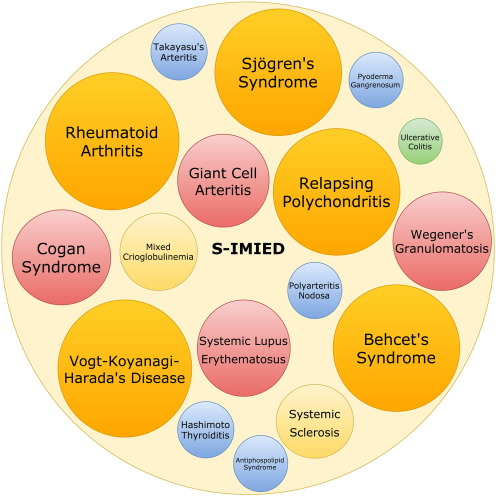
Common Systemic Immune Mediated Inner Ear Diseases (S-IMIED). A few include Sjogren’s (primary symptoms include dry mouth/eyes), rheumatoid arthritis, Behcet’s (blood vessel inflammation), Vogt-Koyanagi-Harada disease (eye inflammation along with neurologic and/or dermatologic involvement), and relapsing polychondritis (cartilage inflammation). Diagnosis can take time and patience due to their fluctuant nature. (Mancini et al., 2018)
What should I do if suspected?
- Refer – Refer patient to a rheumatologist as well as an ENT for additional work-up – The earlier the diagnosis is made, the sooner medication therapy is started, and the better the chance for recovery of inner ear damage (Russo et al., 2018)
- Educate – Once an autoimmune vestibular diagnosis is confirmed, educate the patient using resources like this brochure from VeDA
- Rehab – Treat the patient with appropriate vestibular rehab and balance exercises, particularly using proper VOR adaptation exercises for those with peripheral vestibular involvement
Want to learn more about MS?
We recently reviewed an article by Dr. Graham Cochrane discussing vestibular rehab, fatigue, and MS. Check it our live broadcast from our June Journal Club.

